Infections used to be a greater threat to human life than they now are, with advanced healthcare and public hygiene improvements in Singapore. However, one infection lies literally under our feet and is often underestimated: fungal nail infections.
Fungal nail infections include:
- distal subungual onychomycosis (caused by Trichophyton rubrum, leading to thickened, yellowing, or crumbling nails)
- white superficial onychomycosis (caused by fungi in the nail plate layers, including Trichophyton mentagrophytes)
- candida onychomycosis (caused by candida fungi species infections, often in people whose nails are often exposed to water or previously affected by infections or injury)
- and proximal subungual onychomycosis (usually caused by T. rubrum, often seen in patients affected with HIV with weakened immune systems).
While such infections may not be as life-threatening as some other types of infections, they can be indicators of the overall picture of your health, and affect appearance and confidence. [1]
Dermatologist Dr Liew Hui Min responded to a reader question on treatment methods typically used for fungal nail infections. Here is her detailed response about how dermatologists in Singapore identify and ultimately manage the issue.
What are the common causes of nail infection in Singapore?

Fungal nail infection is the most common nail infection in Singapore. So be careful where you walk barefoot. Walking on dirty surfaces is one cause of fungal nail infections. A visit to the nail salon may also cause an infection if the manicurist does not practice good hygiene.
Trauma to the nails (possibly caused by activities or ill-fitting shoes) and athlete's foot, which may cause infection, are all possibilities. [2]
Nail deformities may not actually be infections
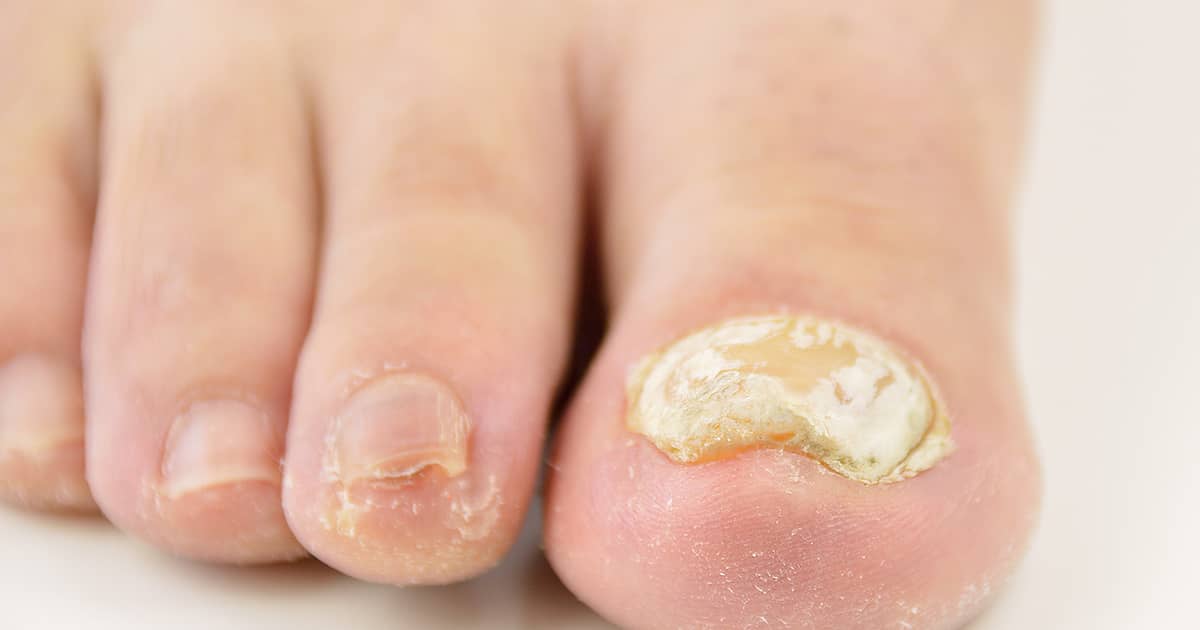
While fungal nail infections can come in various forms, they may also just be nail deformities that somewhat resemble infectious conditions. These are a little trickier to identify, which is why nail clippings are typically sent for a fungal culture to determine if there is a type of fungus or mould present.
Conditions that can be mistaken as fungal nail infections include psoriasis, contact dermatitis, trauma, and yellow nail syndrome. [3]
Results can take up to two months to finalise

Once a sample has been sent to the clinic, it could take up to two months for the culture results to be confirmed. In the meantime, you could try applying topical treatments (like clotrimazole lotion +/- amorolfine lacquer). [4]
Oral antifungals could be solutions to your problem

Once a fungal nail infection has, in fact, been confirmed by your dermatologist, he or she may then discuss the option of using oral antifungals as possible solutions for you.
Oral antifungals are effective but could take at least 3 months or more, which also means costs are considerably high. [5]
There's a possibility that oral antifungals could affect your liver

In addition, oral antifungals could have certain side effects (particularly liver toxicity). This is uncommon, but the possibility is still there, so doctors will need to monitor your liver through blood tests (especially if prolonged treatment is required). [6]
Topical treatments can help, depending on the severity

Due to the factors involved with oral treatment (like price, prolonged application and possible side effects), some people instead only opt for topical treatments when dealing with fungal nail infections.
Their effectiveness, however, depends on the severity of the infection (so you might want to consult your doctor first). [7]
Infections may be followed by pain
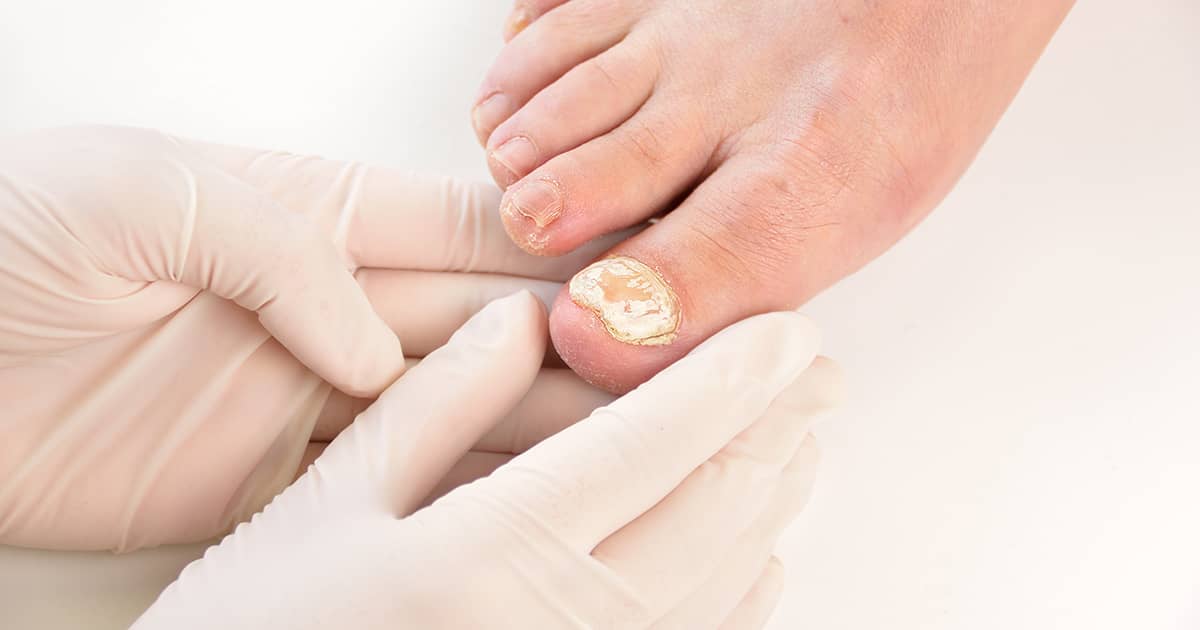
If a fungal nail infection leads to pain, get the nail closely examined to make sure other underlying causes are ruled out. [8]
Consider nail plate removal
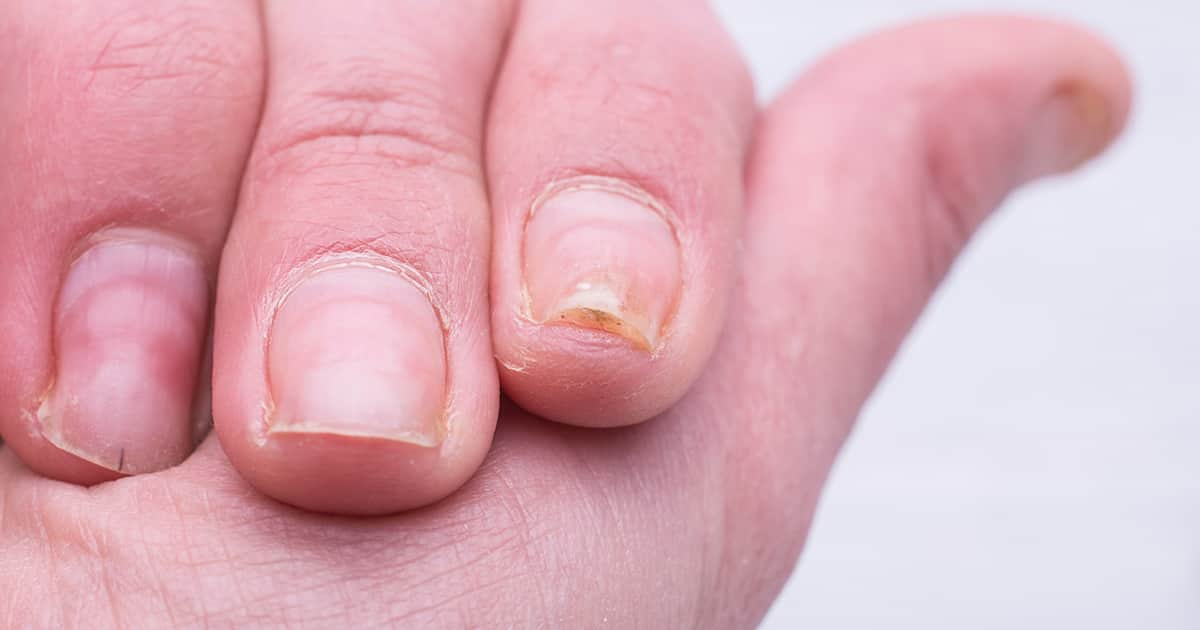
Once a fungal nail infection has been identified and confirmed through thorough assessments, there is an alternative option that could be effective - nail plate removal under local anaesthesia. Once the nail bed starts to heal, topical antifungal medicine can be applied.
If you suspect an infection, it's important that you seek treatment and consultation from a dermatologist before things get worse. There's a possibility that infections could actually be something else entirely so a proper inspection is required.
Would you like to ask any related health questions?
You can Ask A Doctor right away, or view the complete list of Human Sessions.











