Gastroesophageal Reflux Disease, or GERD, is a common digestive condition. It has been gaining attention, especially among the younger generations.
GERD occurs when gastric content frequently flows back up into the oesophagus [1] resulting in a “burning” sensation behind the chest wall. It can also cause severe chest pain and throat discomfort [2].
Depending on the severity of GERD, it may have a big impact on your job and the way you live your life. It is important to find out the extent of injury caused by the acid burn during endoscopy. Your doctor will be able to exclude a premalignant condition known as Barrett’s oesophagus at the same setting [3].
There are a few options available to treat GERD. Patients may simply take over-the-counter remedies or take stronger medications prescribed by their doctor. In extreme cases, surgery may be required. For those diagnosed to have Barrett’s oesophagus, surveillance endoscopy is often recommended.
What exactly is GERD?
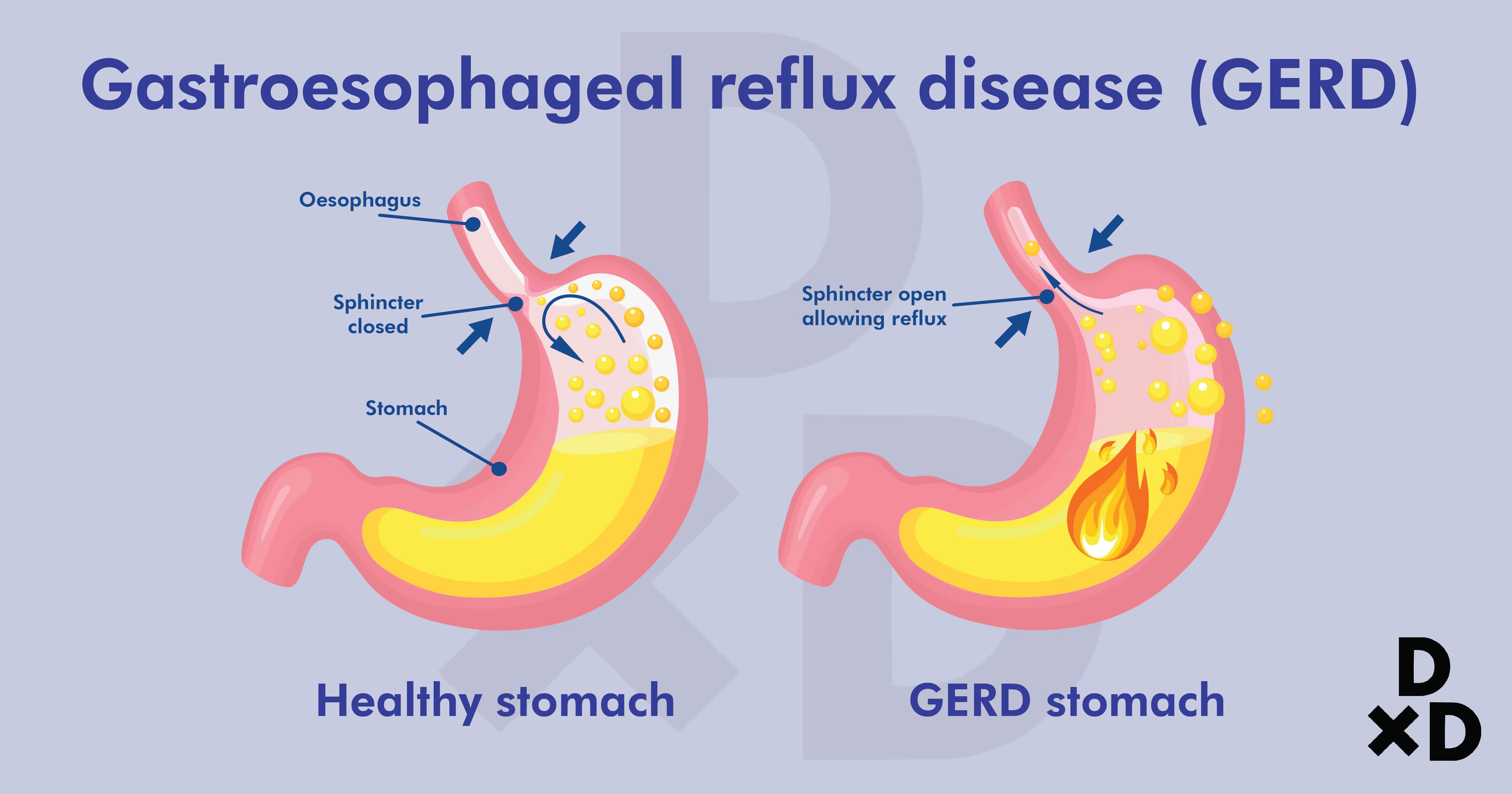
Gastroesophageal reflux disease (GERD) is a prevalent gastrointestinal (GI) condition. In fact, it is one of the most common GI problems faced by digestive specialists in Singapore.
Everyone at some point in time has experienced belching and heartburn. However, people suffering from GERD experience it far more frequently.
Individuals with GERD frequently experience interrupted sleep at night [4]. Their performance at work and social life may also be affected. One major concern of GERD is the formation of oesophageal erosions and ulcers caused by the acid burn [5].
Patients suffering from long-term GERD might also develop a pre-malignant condition known as Barrett’s oesophagus.
What is Barrett's oesophagus?
It is a condition where the cells lining the lower oesophagus change in appearance to resemble those of the stomach and intestine, due to their ongoing exposure to gastric juices [6].
Barrett’s oesophagus is a risk factor for cancer of the lower oesophagus. It is more common in men than in women.
Symptoms of Barrett’s oesophagus are no different from regular heartburn and may seem insignificant. For this reason, many people don’t seek medical treatment until their condition is quite advanced. In fact, most people with cancer of the lower oesophagus have not been previously diagnosed with reflux.
One of the symptoms of GERD is regurgitation, which is an involuntary backflow or reflux of stomach content into the oesophagus.
This reflux usually happens spontaneously without any trigger. It can also occur when performing simple manoeuvres such as bending forward to pick up a coin off the floor. Besides the regurgitation, you may also experience one or more of the following symptoms [7]:
- Heartburn
- Sour or bitter taste in your mouth
- Hoarseness of voice
- Cough
- Having an excessive amount of saliva.
- Heart attack-like chest pains
- Asthma
How did I develop GERD?
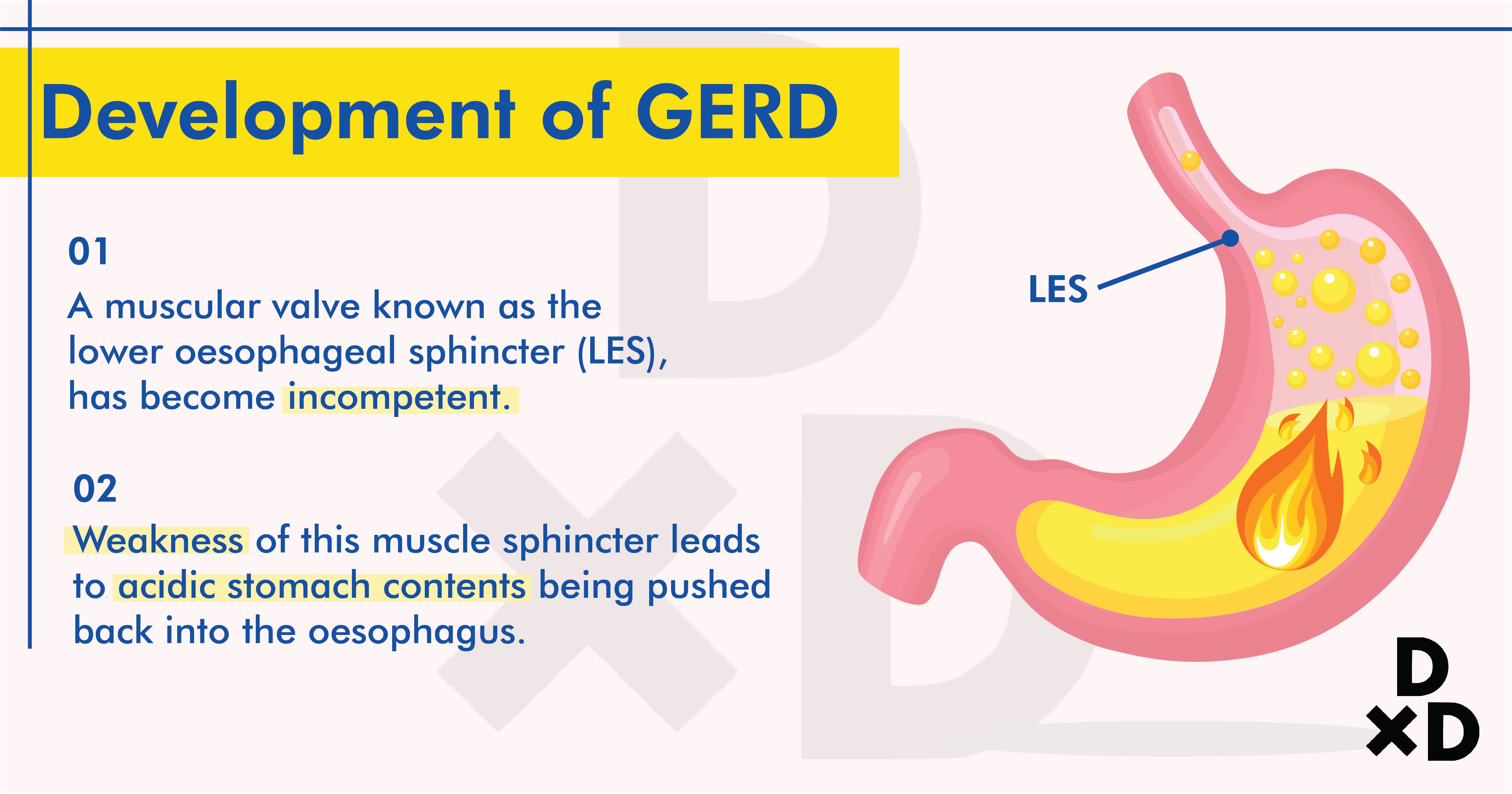
The main reason for gastric contents returning to the oesophagus is an incompetent muscular valve located at the lower end of the oesophagus [7]. This muscular valve is also known as the Lower Oesophageal Sphincter (LES). The sphincter muscles regulate the flow and allow smooth passage of food content from the oesophagus into the stomach in a one-way direction.
Under normal circumstances, the LES is closed and would remain so until you swallow food or liquid.
However, when the muscle sphincter is weak, the acidic contents of the stomach may overcome the sphincter and be pushed back up into the oesophagus. This happens when the stomach contracts or when your abdominal pressure increases as you bend forward to pick things up.
Another reason for gastric reflux is an increase in abdominal pressure. When the abdominal pressure goes beyond a certain level, the LES may transiently relax to allow air to escape. This is otherwise known as belching and it helps in preventing excessive pressure from building up inside the body.
If this pressure builds up repeatedly, the frequency of belching also increases, which may bring along gastric acid that causes heartburn.
Lying down after consuming a heavy meal could also worsen your reflux problem. It is much easier for the acidic liquid to flow across an incompetent valve in a horizontal position.
How to make a diagnosis of GERD?

The most practical way to diagnose GERD is to review your medical history. Typical symptoms of heartburn and regurgitation will provide the basis for diagnosis in most cases.
Chest pain or cough may also be the presenting symptoms of GERD. If these typical symptoms are absent, a short course of medication known as proton pump inhibitors (PPIs) may be given to you to help in the diagnosis [4].
In rare cases, further investigations are needed to confirm the acidic reflux. Some of these assessment methods may be available at your family doctor’s clinic while others require a visit to a specialist.
Besides arriving at the diagnosis, an important finding which affects the management of GERD is the extent of oesophageal injury caused by the acid burn. This information is important in deciding the long-term management plan and the way to use the PPIs.
Unfortunately, the severity and duration of symptoms do not necessarily correlate well with the actual physical injury found in the oesophagus. Patients with severe symptoms may have minimal to no oesophageal injury. On the other hand, patients with mild to minimal symptoms may suffer from injuries such as oesophageal ulcers.
Another challenge we face as digestive specialists is to identify cases which carry a high risk of developing lower oesophageal cancer, otherwise known as Barrett’s oesophagus. This is a pre-malignant condition usually caused by long-term acid exposure.
Gastroscopy procedure
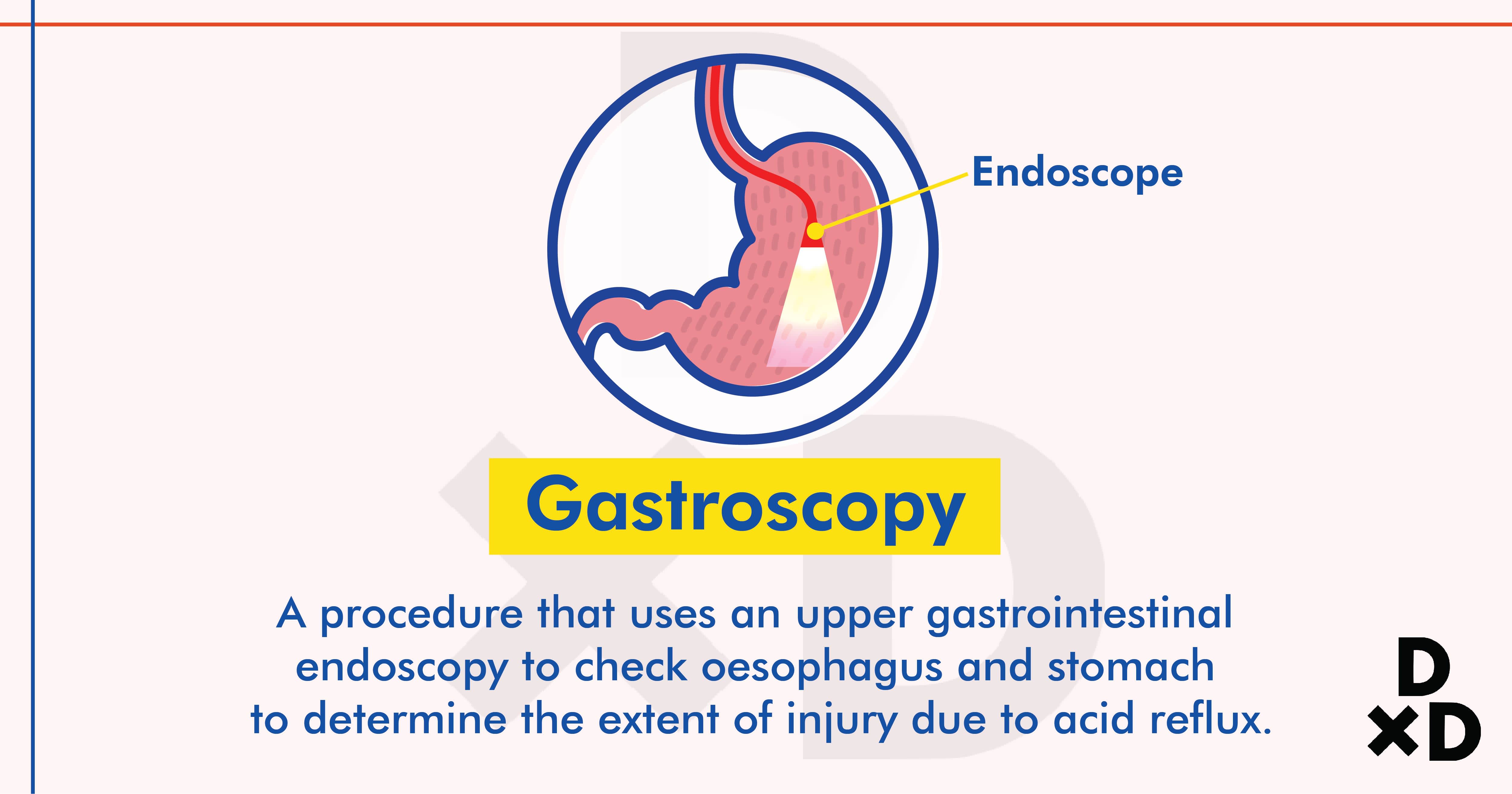
Gastroscopy, or OGD, is a quick and simple procedure. It uses an upper gastrointestinal endoscope to inspect the oesophagus and stomach. The doctor will then be able to evaluate and determine the extent of injury due to acid reflux.
Gastroscopy involves the use of a video endoscope. The endoscope is inserted through your mouth and down your oesophagus into the stomach with direct viewing from a monitor. This procedure carries little risk and can be completed within 5-15 minutes without discomfort [8].
The scope procedure is done under sedation so you most likely will not remember what happened.
Besides checking your oesophagus, stomach and small intestine, the doctor may also collect tissue samples via the scope. He/she would then put them under a microscope for further evaluation.
Through endoscopy, the extent of the injury to the oesophagus and the presence of Barrett’s oesophagus can be confirmed. This information allows the doctor to come up with a management plan for the GERD as well as the surveillance interval to monitor for cancer.
If a special tissue growth, known as a polyp, is found in your stomach, the gastroscopy procedure will most likely be able to remove it without the need for surgery [9].
It is common for patients with GERD to repeat the upper endoscopy and biopsies at regular intervals. This is done to look out for any malignant tissue transformation from Barrett’s oesophagus.
Depending on the clinical findings, it is usually done in intervals of 1 to 3 years. In the event of early cancer changes, endoscopic therapy or surgery may be required as part of the treatment.
When do I need to see a doctor?

This is a very common question raised by people suffering from GERD. My simple answer to this is:
You should visit a doctor whenever you feel that the symptoms are disturbing enough to affect your mood, sleep, job or social life.
Needless to say, you should seek help from your digestive specialist immediately if you experience any of the following worrisome signs or symptoms:
- Recurrent vomiting
- Difficulty in swallowing
- Unexplained weight loss
- Passing out black stools
If you are more conscious about your health and well-being, you are likely to be aware of the many self-assessment applications and online tools available for GERD.
These tools are mostly designed to compare the severity of symptoms during clinic consultation so that you and your doctor can know if the treatment is working well.
However, using the self-assessment method to judge the severity of your GERD based on your symptoms alone is not recommended. Not only is it unreliable and potentially misleading, you may overlook or misinterpret important signs or symptoms which require investigations and further evaluation.
Even among specialists, the complications of GERD cannot be effectively gauged with just your symptoms alone.
%askquestion title=Ask Dr Quan A Question%
How do I get rid of my GERD symptoms?

The primary goal in treating GERD is to reduce the frequency of attacks and preferably to stop all symptoms from appearing altogether. This target is largely achievable despite the fact that it is common to have a recurrence of GERD symptoms. Simple measures such as lifestyle and dietary changes may go a long way.
Lifestyle
Making these small lifestyle changes may help in reducing GERD symptoms:
- Keep an upright posture during meals and for about an hour thereafter
- Consume smaller portions each meal
- Exercise regularly to maintain a healthy body weight
- Elevate the head of the bed when sleeping
- Quit smoking
- Avoid overconsumption of alcohol
- Refrain from eating 2 hours before bedtime
- Wear loose-fitting clothes
Dietary
Adjusting your diet can also help in managing your GERD symptoms. The following are some adjustments you can make:
- Cutting down on foods with high fat content, e.g. fried foods, cream, ice cream, cheeses, sausages, bacon, potato chips, etc. Such foods may delay gastric emptying and decrease the lower oesophageal sphincter (LES) pressure.
- Refraining from eating chocolate and drinking coffee. Both contain methylxanthine, which relaxes the LES pressure. In addition, coffee can induce more acid production in the stomach which may worsen the sensation of heartburn during regurgitation.
- Avoiding alcohol, peppermint, citrus, tomatoes, and/or carbonated beverages if your symptoms are bad. These foods may irritate your oesophagus directly or worsen your symptoms of gastric reflux.
Medication
Despite taking the necessary precautions and heeding all advice on diet and lifestyle changes, there will still be a few out there who will continue to experience significant GERD symptoms. This may be the time when medicine comes in handy.
Over-the-counter medications such as antacids can be effective in overcoming mild symptoms. This treatment is readily available at most local pharmacies. Prescription is not required for these over-the-counter medications. In more established cases, specific acid suppression therapy such as H2-blockers and Proton Pump Inhibitors (PPIs) will be required to lower the acidity in the refluxate from your stomach [7].
Such treatment is usually given for a short period of time when your symptoms flare up. In fact, on-demand PPIs treatment driven by symptoms is a common strategy adopted by healthcare professionals worldwide.
The downside to this strategy, particularly in Singapore, is that you will need a prescription from your doctor. In more advanced cases, long-term medicine or even surgery may be required to relieve symptoms and prevent further complications.
I would like to stress that getting rid of the symptoms, although important to you, is only one facet of the overall management of GERD. Another important aspect you should know is whether you have developed any of these complications in your oesophagus:
- Bleeding
- Ulcers
- Scarring
Such complications may give rise to swallowing problems in future. For those who have been diagnosed to have Barrett’s changes due to acid reflux, cancer surveillance at suitable intervals would be highly recommended.
Can GERD be cured permanently?
There are many reasons why the LES does not behave normally as a one-way valve should. Some of these factors are not permanent. As such, the GERD symptoms may improve over time or even resolve completely when these factors no longer exist.
A typical example is obesity or pregnancy. The high intra-abdominal pressure present in this case may increase the frequency of acid reflux. When the same person manages to lose weight, the pressure in the abdomen reduces and so will the GERD symptoms.
For GERD due to issues innate to the sphincter muscle itself, it is less likely that the symptoms will go away completely. However, these symptoms can still be effectively managed if you pay close attention to your diet and lifestyle. There are many who require medication from time to time with a handful that may need to take medication on a daily basis.
Should I undergo surgery to treat my GERD?
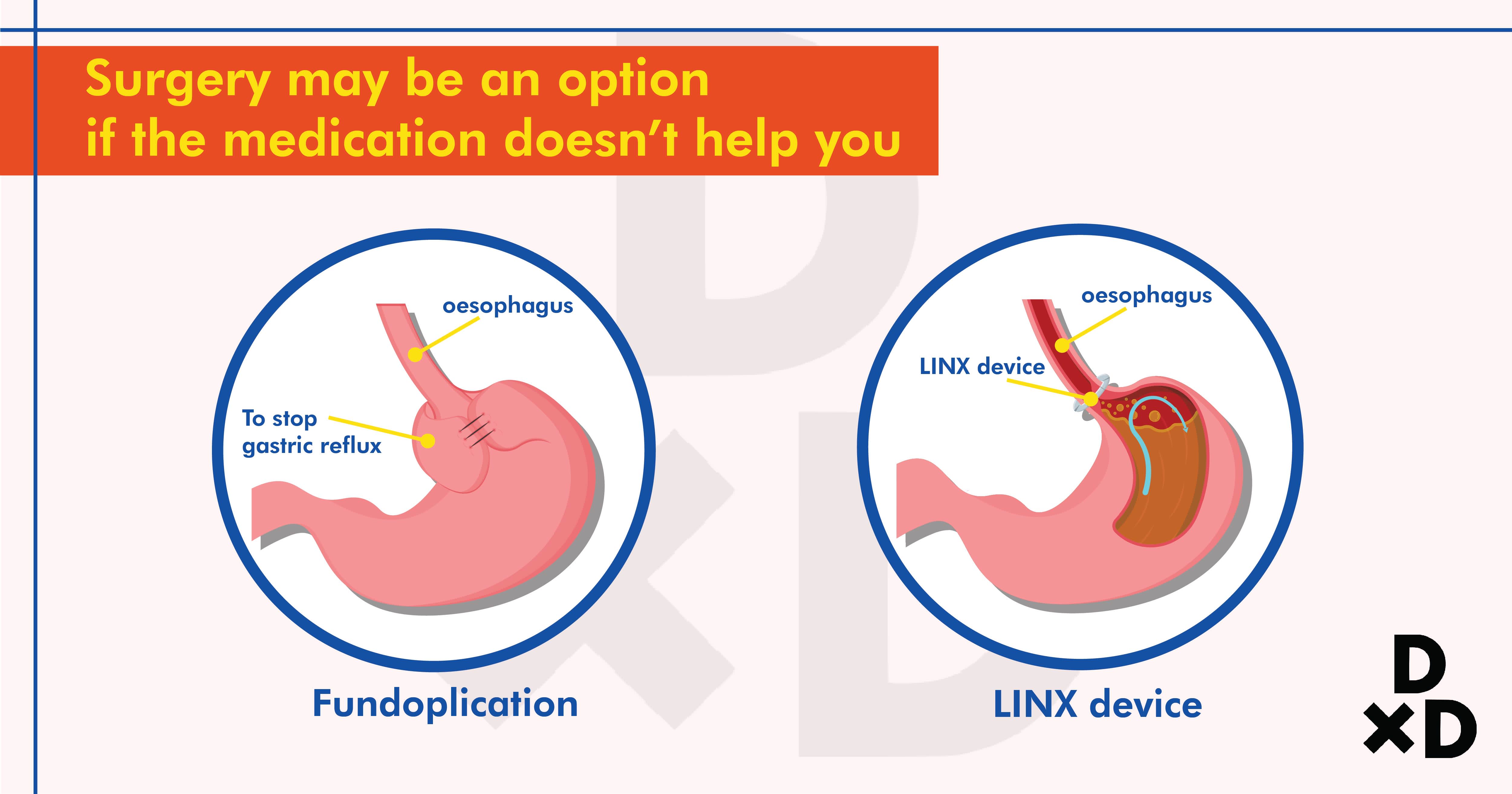
When your GERD symptoms are not well controlled or when the medication prescribed by your doctor is ineffective, surgery may be your next option. In general, surgery is reserved for burns or ulcers in the oesophagus or when cancer has developed in your oesophagus.
This is because surgery comes with its own set of risks and complications. It should only be considered when the benefits you may get outweigh the risks that you have to undertake.
In addition, it has been shown that people with GERD symptoms who do not respond well to PPIs also responds poorly to surgery. As such, I urge you to discuss the risks and benefits with your digestive specialist and understand exactly what you will be going through before undergoing any surgery.
The more common surgical option involves tightening the LES and repairing the function of the valve. This is known as fundoplication. There are different techniques to achieve this and they all share the same effect of reducing or stopping gastric reflux [10].
One of the newer methods is to surgically insert a ring of magnetic beads around the lower oesophagus. This enhances the sphincter function [11]. The attraction between these beads effectively forms an elastic band around the oesophagus, thereby reducing the chance of regurgitation.
%bookappointment title=Book Appointment With Dr Quan%
Conclusion
GERD is a common problem in Singapore and is on the rise. Change in dietary habits and lifestyle can help to reduce the recurrence of GERD symptoms.
The appropriate use of medicine under the supervision of healthcare providers has been shown to be a safe and effective way for most established cases. Do watch out for suspicious or alarming signs and seek medical help early.
A gastroscopy may help in confirming the presence of erosions, ulcers as well as Barrett’s changes at the lower oesophagus. It is also a valuable tool for cancer surveillance at suitable intervals. Surgery, although rarely required, may be an important option to tackle severe and complicated GERD, especially when medical therapy fails.
%treatmentquote title=Get treatment quote for Gastroenterology%
Dr Quan Wai Leong, as the Director of Endoscopy Centre, founded the computerised simulation training service in endoscopy at Tan Tock Seng Hospital. He introduced SpyGlass cholangioscopy system in Singapore to treat large bile duct stones and manage difficult strictures.
Read more of Dr Quan Wai Leong's QnA here.
Would you like to ask any related health questions?
You can Ask A Doctor right away, or request for treatment quotes from doctors.












