Most of us don’t realise the importance of our urological health.
Your urinary tract filters waste from your bloodstream and expel them from your body along with excess fluid as urine, so a healthy urinary tract is vital for maintaining your physical well-being.
Having healthy kidneys, which are part of the urinary tract, helps to:
- prevent metabolic waste products from building up
- remove excess fluids in your body
- maintain the balance of electrolytes
- produce hormones that help regulate blood pressure
- make red blood cells
- keep bones strong
As our urinary tract plays such important functions, we cannot afford to take it for granted.
However, urinary tract infections (UTIs) can still happen even if you have done all that you could do to prevent it. You may then start wondering:
- Who should I see?
- At what point should I see them?
- What happens when I see them?
In this article, I will be covering all your doubts about seeing a urologist. Hopefully, after reading this article, you can make the most informed decision when it comes to your urological health!
Firstly, what is a urologist?
A urologist specialises in diagnosing and treating diseases of the urinary tract and male reproductive system [1].
What do urologists treat?
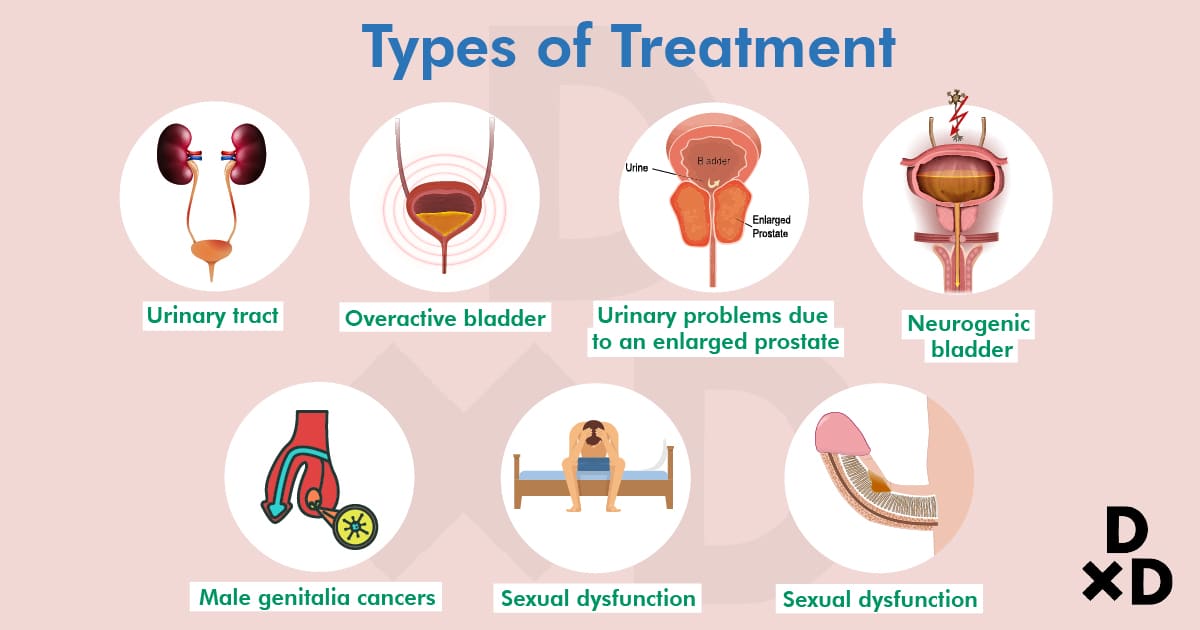
As stated above, a urologist treats a wide range of conditions [2]. Here are a few that affect the urinary tract or system:
urinary tract
stone diseases — stones in the kidneys, ureters, bladder
infections — pyelonephritis, cystitis, prostatitis
cancers — kidney cancer, ureteric cancer, bladder cancer, prostate cancer
urinary problems due to an enlarged prostate, such as benign prostatic hypertrophy
overactive bladder
neurogenic bladder
Besides that, they also treat problems that affect the male reproductive system, including but not limited to:
- male genitalia cancers — testicular cancer, penile cancer
- sexual dysfunction — ejaculatory disorders, erectile dysfunction
- male fertility issues
- disorders of the penis — congenital penile curvatures, phimosis or tight foreskin, Peyronie’s disease
Are there sex-specific urologists?
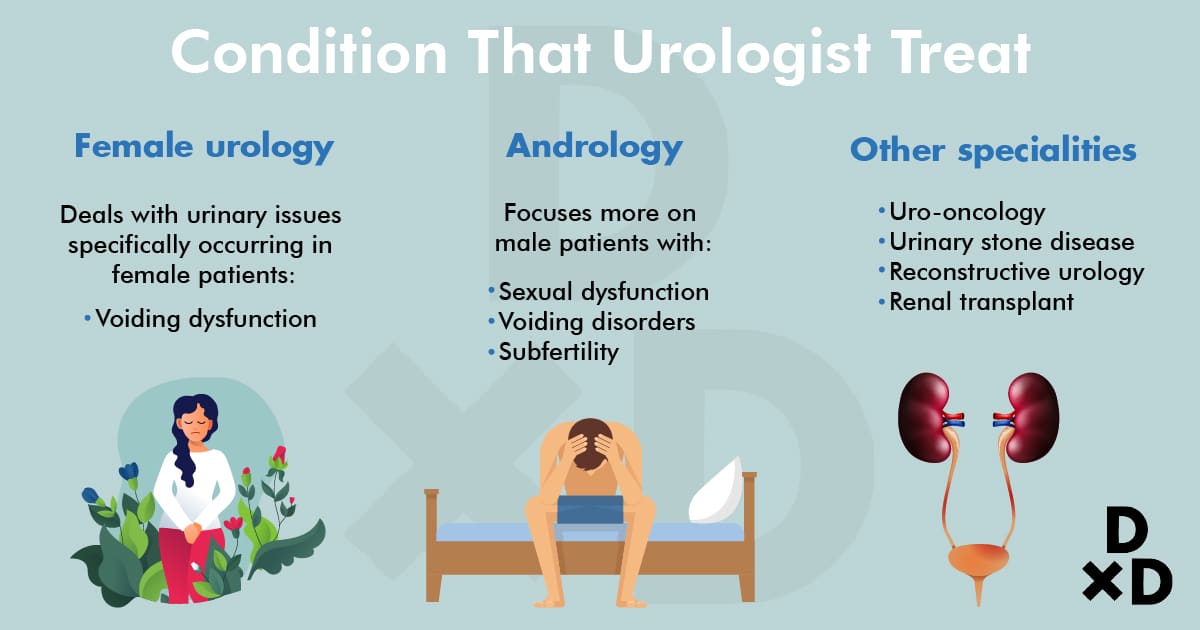
In general, urologists can advise patients of both sexes. However, some of us do have further sub-specialities. Here are the sub-specialities that are sex-specific:
Female urology
This does not refer to the urologist being female. Those in this sub-speciality deal with urinary issues specifically occurring in female patients.
Thus, they tend to be better versed in dealing with functional urology issues such as voiding dysfunction.
Andrology
Andrologists focus more on male patients with:
- sexual dysfunction
- voiding disorders — most commonly benign prostatic hyperplasia (BPH)
- subfertility
Some andrologists can also be prosthetic urologists. These doctors are knowledgeable about penile implants and urethral slings. They use implants and slings to treat:
- erectile dysfunction
- penile curvatures
- male urinary incontinence
Other specialities
Besides that, there are many other specialities such as:
- Uro-oncology (cancers of the urinary tract and male genitalia)
- Urinary stone disease
- Reconstructive urology
- Renal transplants
If you are unsure which sub-specialist you should be seeing for your condition, you may consult a general urologist, who would be able to access your condition and refer you accordingly.
What special training do urologists have to go through? Is there a special certification?
A urologist is basically a surgeon. Hence, a urologist would undergo general surgical training before embarking on this sub-speciality training.
In Singapore, doctors specialising in urology will undergo a 6-year urology residency programme at the restructured hospitals.
All specialist trainees would have to take post-graduate exams as determined by each training programme. The exams are conducted annually before the conclusion of the programme.
Upon passing the Nationwide Exit Certification at the end of the specialist training, the Specialist Accreditation Board will register the doctor as a specialist urologist with Singapore's Ministry of Health.
Those who want to sub-specialise further then go for fellowship training after being registered as a specialist urologist.
How are a nephrologist and a urologist different? How do I know whom to consult?
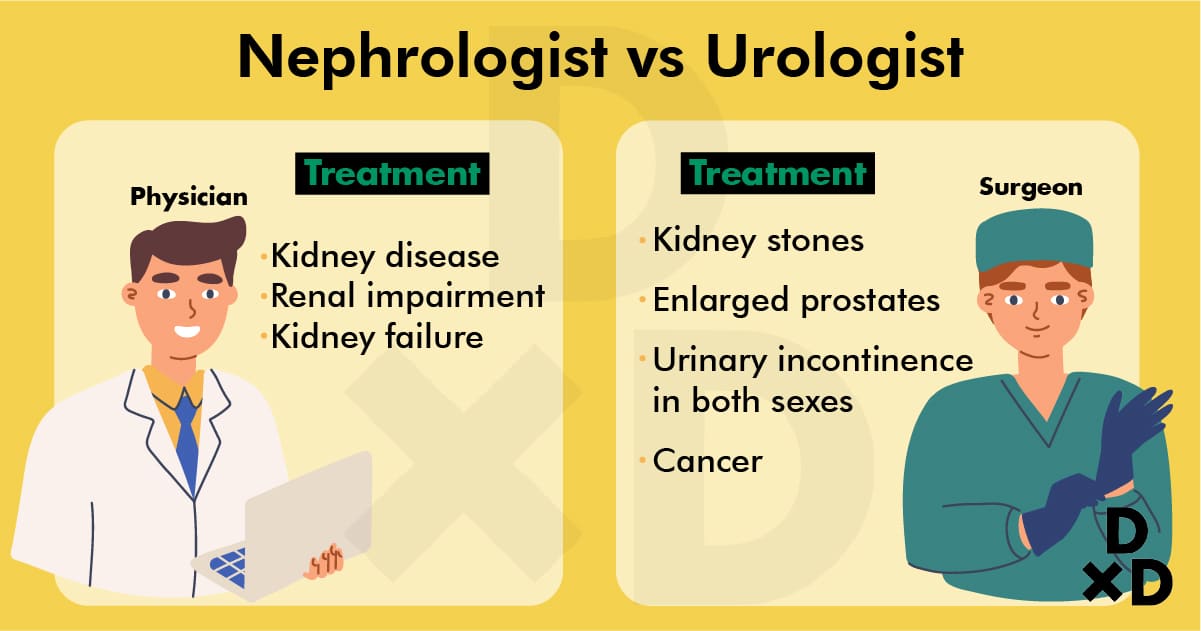
Simply put, a urologist is a surgeon, while a nephrologist is a physician.
Urologists take care of conditions affecting both the male genitalia as well as the reproductive system. Furthermore, we take care of problems that affect the urinary system in both sexes.
Some common problems that warrant a visit to the urologist include:
- kidney stones
- enlarged prostates causing urinary symptoms
- urinary incontinence in both sexes
Besides that, we also treat cancers of the:
- prostate
- kidneys
- bladder
- testicles
We operate on these patients using open surgical techniques as well as minimally invasive techniques such as laparoscopic keyhole surgeries. For some conditions, these keyhole surgeries are robot-assisted.
Male subfertility issues, as well as sexual dysfunction in men, are also issues that urologists treat. Some urologists are also renal transplant surgeons.
Nephrologists, or renal physicians, are internal medicine specialists. They deal with patients with kidney disease, renal impairment and kidney failure.
However, it is not uncommon for a urologist to work together with a nephrologist. We believe that by doing so, the patients will benefit from the combined expertise.
If you are still unsure, be sure to visit a doctor for a consultation.
What are some common illnesses you see in your practice?
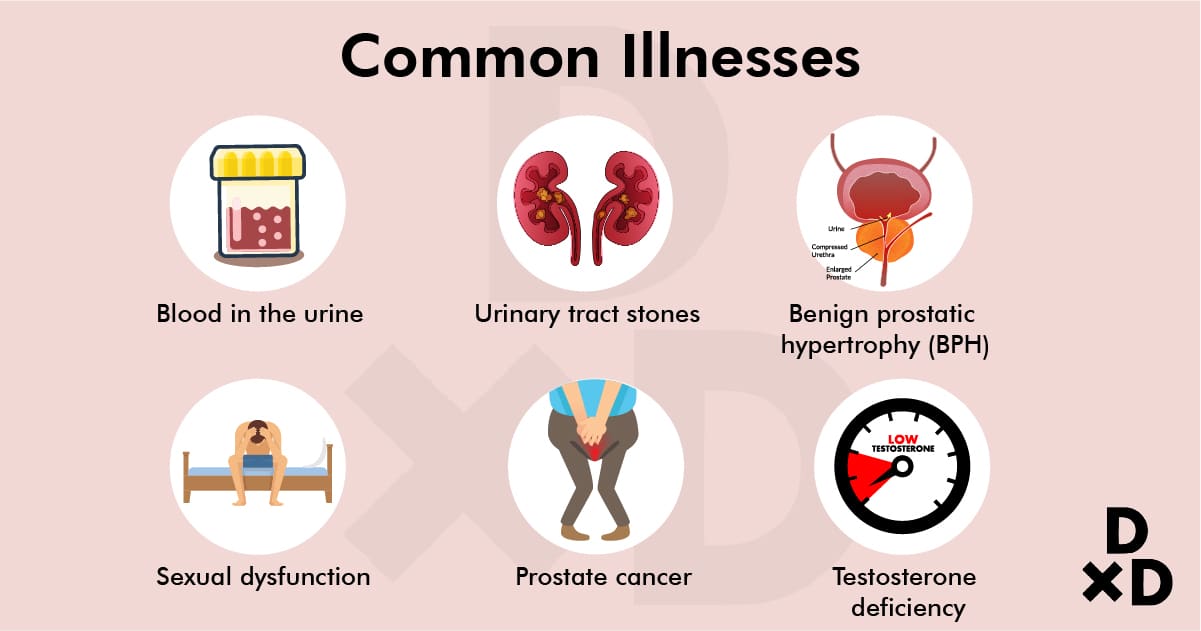
In my years of practice, here are some of the common diseases and disorders that I often see:
Blood in the urine
The medical term for blood in urine is haematuria. In haematuria, your kidneys or parts of your urinary tract allow blood cells to leak into the urine.
It is often painless. However, at times, it can be painful and comes with various other symptoms.
Read more here: Complete Guide To The Causes Of Blood In Urine In Males & Females (2020)
Urinary tract stones
Stones are basically large crystals that can be found anywhere along the urinary tract, be it the urinary bladder, kidneys, ureters or urethra.
Stones can cause bleeding or infection. Depending on their location, they may block the flow of urine causing colic, or pain. Patients with urinary tract stones either report pain, or the stones are picked up incidentally during health screening scans.
Benign prostatic hypertrophy
Also known as prostate gland enlargement, BPH commonly occurs in men as they get older, especially for those above the age of 50.
Patients often experience disturbances when they go to the loo. The condition causes uncomfortable symptoms such as [3]:
- slow urinary stream
- straining to empty the bladder
- waking up at night to pass urine
- frequent urge to urinate
Read more here: Managing Benign Prostate Hyperplasia & Peyronie’s Disease: A Urologist Discusses
Sexual dysfunction
Examples of sexual dysfunction include premature ejaculation, erectile dysfunction (ED), penile deformities. These conditions also affect the patient's partner negatively during sexual intercourse.
ED is more common in men above 50, but it can occur at any age. In the past 5 years, I have noticed that more younger men are coming forward to seek medical attention for this problem.
Contrary to popular belief, ED is not always due to ageing [4].
Read more here: Your Essential Guide To Erectile Dysfunction Treatment In Singapore
Prostate cancer
The risk of BPH increases as a man ages. Similarly, the risk of prostate cancer increases, and in fact, both conditions can co-exist!
Having BPH does not exclude you from having prostate cancer. As the prostate gland is an organ that has a sexual function, treatment of prostate cancer does not end at remission of the disease.
More often than not, the urologist would have to take into consideration the cancer survivor’s expectations. This could be in terms of urinary function and sexual function.
Read more here: The Ultimate Guide in Dealing with Prostate Cancer By a Singaporean Urologist (2020)
Testosterone deficiency
Men with testosterone deficiency often present with:
- low energy levels
- decreased sexual desire
- erectile dysfunction
In addition to these symptoms, the patient's blood testosterone level will be under the lower limit.
Due to the sexual problems associated with this condition, the man’s partner is also affected, and his relationship may suffer.
Testosterone treatment does not involve the abuse of anabolic steroids. It is a treatment for a true clinical condition involving a long-misunderstood hormone.
Read more: Are You Testosterone Deficient?
What urology-related trends do you see happening in Singapore?
The general public is now more aware of urological diseases such as prostate and testicular cancers, thanks to the more frequent conducting of public awareness talks. The Internet has also made the search for medical information easier.
Compared with the past, men are also more willing to come forward when they have issues in the bedroom. Now, they know that these conditions are potentially treatable! They also know where to get treatment legitimately instead of relying on unprescribed potentially fatal drugs from back alleys.
With regards to the treatment in general, the majority of sufferers are not just looking for disease control alone, but also consider the possible side effects as well as risks.
In the treatment of urological disease, there are potential repercussions for sexual function. This is because the urinary tract is intimately related to the genitalia, especially for men.
One example would be in the treatment of lower urinary tract symptoms due to BPH. In order to improve urinary flow in men, doctors will suggest medications and even surgical treatments. However, these treatments can result in sexual dysfunctions like retrograde ejaculation and erectile dysfunction.
Despite that, there have been newer minimally invasive treatment options available in recent years. These options are better for those who want to preserve their sexual function.
When should I visit a urologist?
If you have one or more of these problems, you should have a doctor take a look:
- blood or traces of blood in your urine
- problems passing urine
- pain during urination
- back pain from suspected kidney stones
- problems with conceiving (and a desire to determine if it is an issue with the man)
- problems performing in the bedroom
This is not an exhaustive list, but do make an appointment with a urologist if you face any of these issues.
What are some urology tests?
Uroflowmetry (UF)
Uroflowmetry is one of the specialised tests conducted by all urology clinics. Often called a uroflow test, it is a standard diagnostic tool [5] used to measure the speed of urination.
The doctor will recommend a uroflow test if you have one of these symptoms:
- weak urination
- slow urine stream
- difficulty in urinating
The results from the test would give the urologist an idea if there is a likely blockage in the urethra or the prostate, and if there is significant urine left in the bladder after the patient completes the act of passing urine.
Sometimes the test can suggest if the bladder is “weak”, where the contraction of the bladder during voiding is impaired. If the findings need further evaluation and confirmation, a urodynamics study will be performed.
Urodynamics study (UDS)
The UDS is a more invasive and detailed study. It helps determine the:
- speed of urinary flow
- urinary bladder function in terms of holding urine
- voiding urine
- urinary continence
- other disturbances of the bladder function
Ultrasound scans
Ultrasound scans are commonly performed in an outpatient clinic setting. Therefore, it is able to aid in the quick diagnosis of the problem.
Scans are like an extension of a clinical examination, allowing us to look into the body. CT scans and MRI scans are be ordered when your doctor feels that they are required.
Cystoscopy
Cystoscopy, also known as a bladder scope, involves inserting a flexible scope with a camera at its tip into the urinary tract. From there, your doctor will be able to survey the:
- urethra
- prostate (for male patients)
- bladder
What treatments do urologists perform?
Several urology treatments are available:
- open surgery
- laparoscopic surgeries (key-hole) with or without robot assistance
- microsurgical surgery
- endoscopic surgery (using scopes inserted in the urinary tract)
- extracorporeal shockwave treatments (delivering shocks into the body e.g. ESWL for stone treatment, ESWT for treatment of chronic pelvic pain and erectile dysfunction)
MOH pricing
As per Singapore's Ministry of Health (MOH), here are some prices for the commonly performed bladder scope procedure.
The prices are based on past transaction fees, so this serves only as a guide. Do note that bladder scopes are typically performed in the clinic or as a day surgery procedure.
Bladder scope (with or without biopsy)
Type
Price range
Public, unsubsidised
$626 - $889
Private Day Surgery
$1,826 - $3,270
Private Clinic
$1,284 - $1,953
Do note that for private hospitals, 25% of patients are charged lower than the lower bound and 75% of patients are charged lower than the upper bound.
Public hospitals get subvention from MOH, so their price ranges would seem lower than those of private hospitals.
It is best that you check with and consult your urologist regarding prices as there are many variables. It is very important to note that the prices are heavily dependant on various factors such as:
- experience and knowledge of the doctor
- complexity of case
- where the procedure takes place
What can I expect on the first visit to a urologist?

When you are visiting a urologist, you should come with a full bladder. More often than not, the urologist would need a urine sample from you. This is especially so if you are coming in due to urinary symptoms.
In addition, the urologist would get your history and conduct a physical examination. Some of us would even proceed with ultrasound scans in the consultation room to aid in the diagnosis of your problem.
Urine tests, blood tests and other more specialised imaging such as X-rays, CT scans and MRI will also be taken when necessary.
It is important to work together with your urologist in addressing your problems, as that will allow your doctor to recommend a treatment option. It will also help ensure the suggested option is suitable for you.
Conclusion
You should take a trip down to a urologist if you:
- experience pain during urination
- see blood in your urine
- experience sexual issues — including trouble conceiving or performing
Visiting a urologist is nothing to be ashamed of. Taking care of your urological health is just as important as taking care of the other aspects of your health!
Dr Ronny Tan is a consultant urologist and andrologist who is practicing at Advanced Urology. Dr Tan is also a Fellow of the Academy of Medicine, Singapore. He received his fellowship training in his area of specialty in the USA, as well as an SMSNA (Sexual Medicine Society of North America)-accredited clinical fellowship in Tulane University, New Orleans.
Read more of Dr Ronny Tan's Q&A here.

