Vitiligo is an acquired skin condition where areas of the skin lose their pigment over time, resulting in the formation of white patches on the skin. Famous personalities living with vitiligo include Winnie Harlow (of America’s Next Top Model fame), Joe Rogan, Amitabh Bachchan, and most notably, of course, Michael Jackson.
This is not a rare condition. In fact, as many as one in 100 people are estimated to be living with vitiligo. However, even though vitiligo is relatively common in our population, there are large gaps in knowledge regarding the condition in Singapore and Asia.
As a doctor who focuses on treating patients with vitiligo, I decided to write a guide to share my experiences. I will touch on the condition, how it is managed in Singapore, and methods with which people living with vitiligo can improve and maintain the health of not just their skin, but also their overall physical wellness.
What is vitiligo and what causes it?
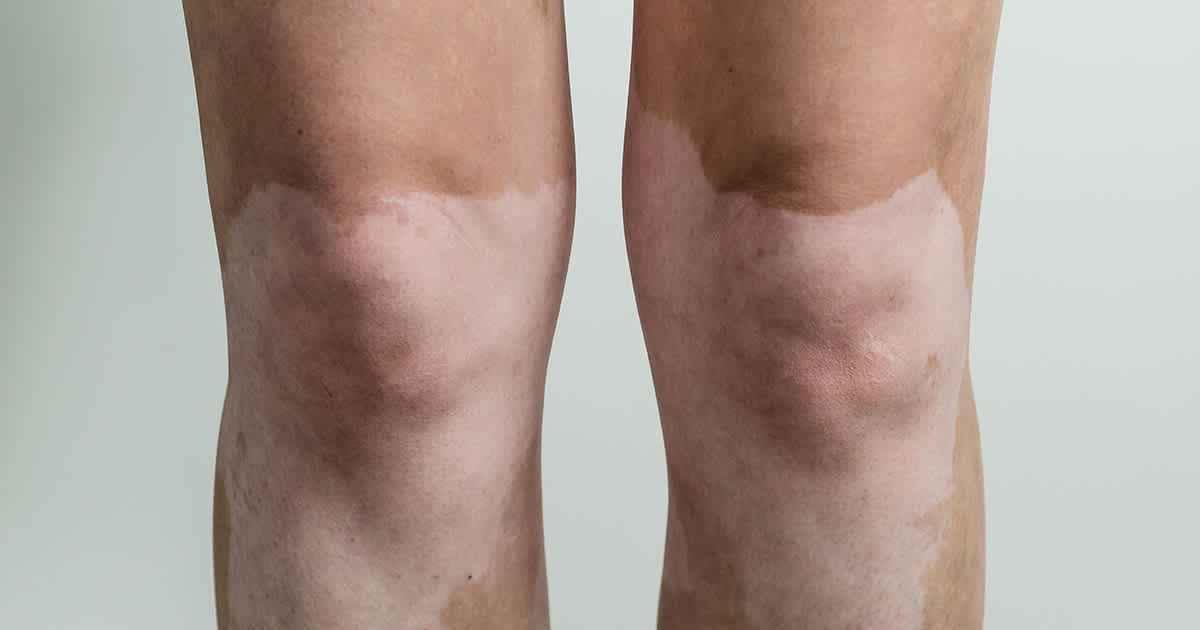
Simply speaking, vitiligo is an acquired depigmentation of the skin.
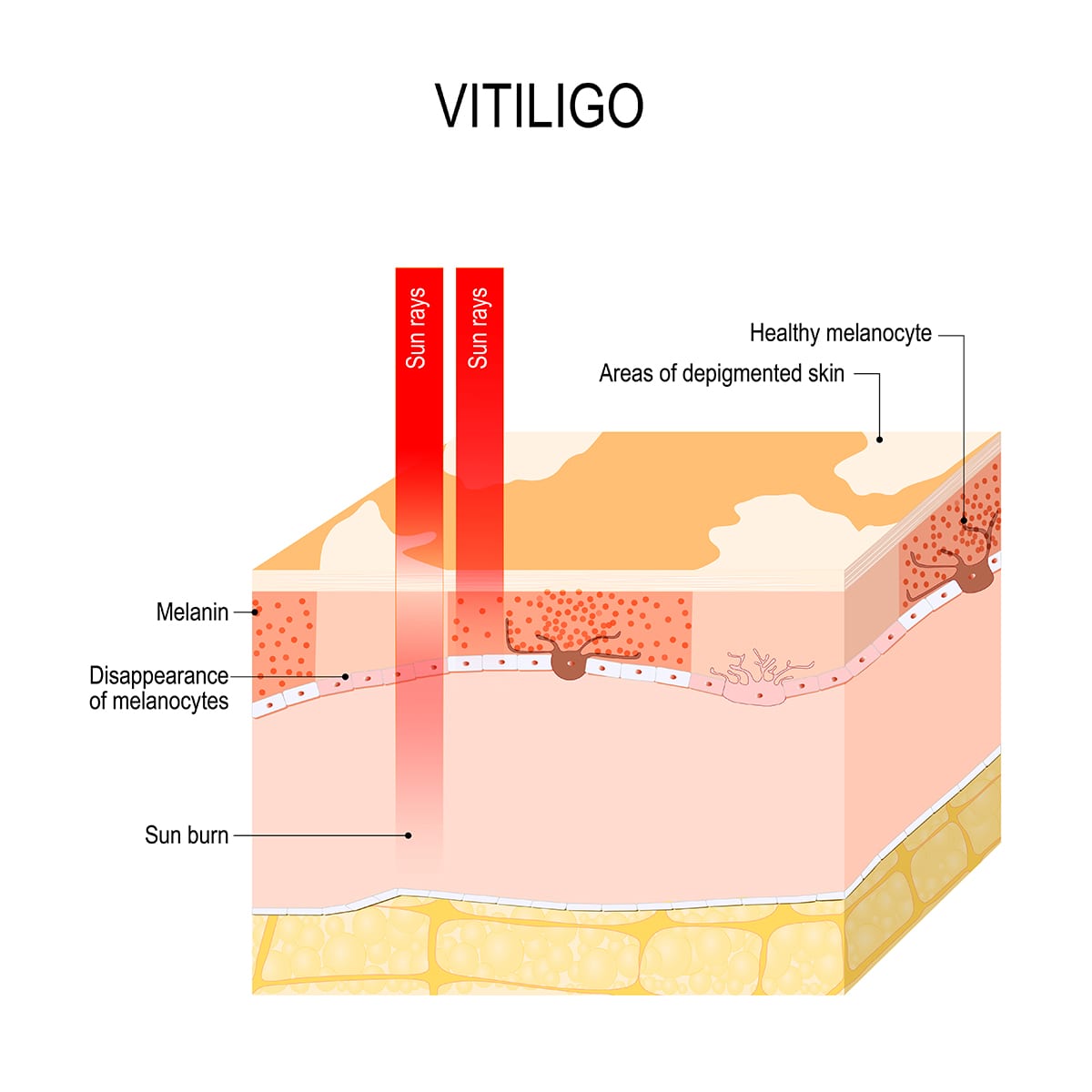
While the exact underlying cause of vitiligo is less well understood, it is widely understood to be caused by immune cells targeting and destroying the pigment-producing cells of the skin.
These pigment-producing skin cells are also called melanocytes. As melanocytes are destroyed, the patient experiences a gradual loss of skin pigment until there is a white appearance that we see in vitiligo-affected skin. This process can happen in one or multiple areas covering the body. [1]
What are the symptoms of vitiligo?
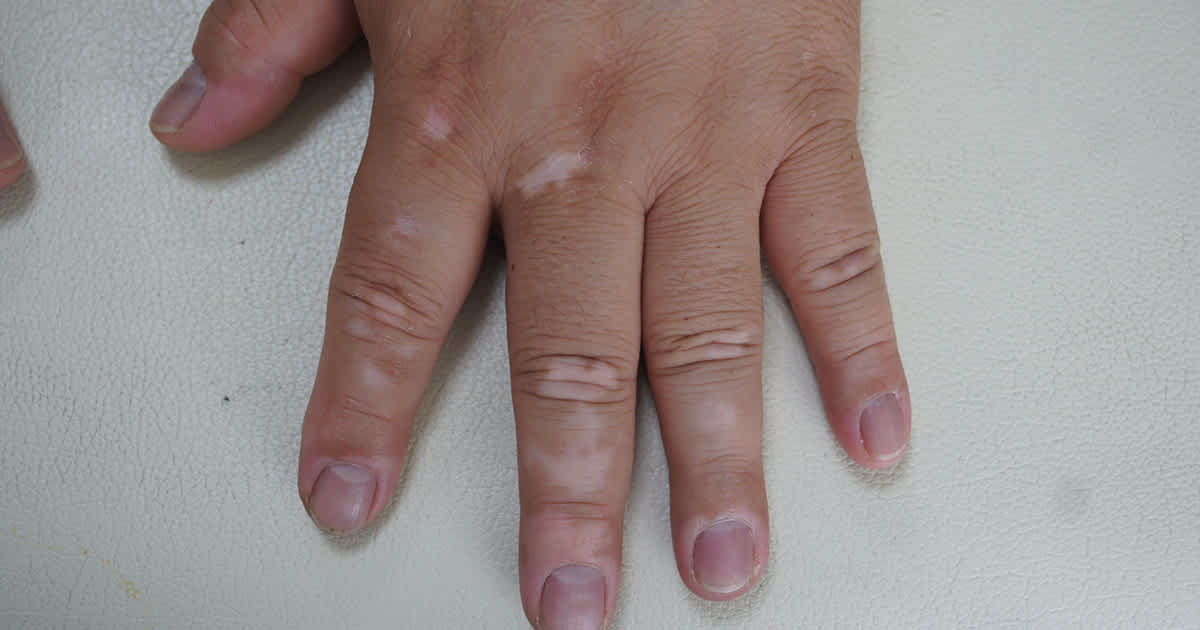
Strictly speaking, vitiligo is a cosmetic condition which is non-contagious and does not have any associated symptoms of itch or pain. However for patients living with the condition, it may have far-reaching implications. The altered appearance can affect an individual’s confidence, social interactions, love life, and even career prospects, to name a few.
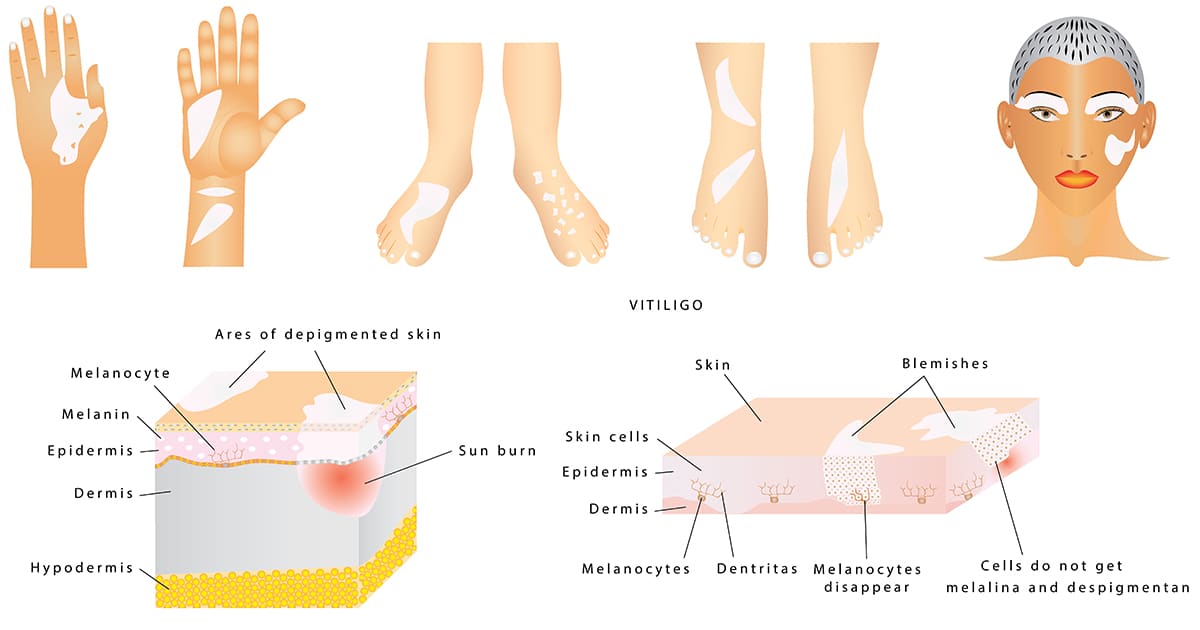
White patches on the skin caused by vitiligo can occur around the:
- hands and feet
- arms and legs
- face and lips
- armpits and groin area near the hip
- around the mouth, nose, and eyes
- inside the mouth and on the inner lips
- belly, and
- genital and rectal areas [2]
Vitiligo can also cause hair growing out of affected areas to turn white prematurely.
Wasn't there a famous celebrity with vitiligo?

Yes. The most famous celebrity who lived with vitiligo is Michael Jackson, the king of pop. Some have suspected that he underwent skin bleaching. He had said in interviews that he sought lightening makeup for the darker patches of his skin to even out its appearance.
After his death, hydroquinone and benoquin were also found in his mansion. These are prescription topical medicines used to lighten parts of skin that have not been depigmented by vitiligo. [3] These are different from skin bleaching.
Michael Jackson was often misunderstood as trying to look as if he was from a different race. It is now known that he was proud of being of African-American heritage, and that vitiligo has no connection to one’s ethnicity and how one identifies with it. In the same way, having any other kind of medical condition does not change one’s ethnicity or DNA.
The anniversary of Jackson’s death, 25 June, is now known as World Vitiligo Day.
If you want to learn more about how Michael Jackson coped with Vitiligo and his general history of health problems, this Wikipedia article provides very objective and well-researched information.
Another celebrity living with vitiligo is Winnie Harlow, known from America's Next Top Model. She was bullied in school and switched schools several times due to her condition, and was discovered by Tyra Banks on Instagram before participating in the show that brought her to fame. She has commented on press coverage that portrayed her as a “sufferer” of vitiligo:
I’m not a “vitiligo sufferer”. I’m not a “vitiligo model”. I am Winnie. I am a model. And I happen to have vitiligo. Stop putting these titles on me or anyone else.
Harlow has received the honour of BBC's 100 Women in 2016 and has starred in many magazine and advertising campaigns.
What are the most common misconceptions about vitiligo?
Here are some myths and facts about vitiligo to address common misconceptions people have about the condition. I hope information like this can help to destigmatise the condition.
Myth: Vitiligo is infectious.
Fact: Vitiligo is not an infectious disease. You can shake hands, hug, and share food and drinks with a person living with vitiligo without contracting the disease.
Myth: Vitiligo is caused by having parents of two different races or who are mixed-race.
Fact: Vitiligo is not related to the ethnicity or heritage of either of one's biological parents. In fact, people with vitiligo may have even skin pigmentation (which is socially considered as "normal") as a child.
Myth: Only people with darker skin get vitiligo.
Fact: Vitiligo can affect people with all kinds of skin tones. It is simply more visually apparent in a person with darker skin.
Myth: Vitiligo can get worse when you eat or drink certain food and drinks, such as white foods like milk and cheese.
Fact: There is no strong evidence to suggest that any specific foods can affect the progress of vitiligo. Do note that a healthy and balanced diet is important with building a strong immune system to cope with any disease.
Myth: People with vitiligo are less intelligent.
Fact: Vitiligo does not cause any mental disabilities or differences in mental or academic performance. Even the mere suggestion of it is absurd.
Myth: Vitiligo is the same as albinism, leprosy, and skin cancer.
Fact: Vitiligo belongs to a family of hypo/depigmentation disorders. While it may appear similar to albinism, leprosy or certain subtypes of skin cancer, there are crucial differences which hold it apart from them.
Myth: Sun exposure causes vitiligo.
Fact: There are no direct links to suggest that sun exposure causes vitiligo. While the appearance of vitiligo can be made worse by sun exposure, it would be incorrect to say that it is caused by sun.
Who is more likely to get vitiligo?

Vitiligo occurs in people of all ethnicities and skin colours, but can be more noticeable on people with darker skin. It can happen at any age, though it has the highest chance of developing from ages 10-30.
Vitiligo has a tendency to occur more among patients with:
- concurrent autoimmune conditions such as thyroid disease and type I diabetes.
- It may also occur in relation to trauma to the skin, cuts, and bruises,
- or even sunburn and friction.
These may all predispose or trigger the development of vitiligo.
Another potential trigger is exposure to certain industrial chemicals containing phenols. I have had a number of my patients who found that their condition flared during periods of intense stress.
These triggers and associations help to underscore that vitiligo treatment is not straightforward. It requires a holistic examination and approach to properly address the condition. [4]
Is vitiligo hereditary?

Vitiligo may be genetic as it is known to happen within families. I have had patients who found that many of their first-degree relatives have had vitiligo in some shape or form.
However, genetics do not account for the whole story. As mentioned earlier, there may be a genetic tendency to form vitiligo. But unless the other conditions are met (such as trauma or stress), some people with strong family backgrounds may never develop the condition.
For example, a pair of twins may have identical genetic makeup, but only one might develop vitiligo in their lifetime. It is estimated that only 23% of twins both develop vitiligo in a lifetime.
Rather than calling vitiligo hereditary, I would say that the tendency to develop vitiligo can be hereditary. [5]
Can vitiligo go away by itself?

It is possible for patches of vitiligo to disappear on their own. To be more accurate, your pigment-producing cells may continue to multiply by themselves and repopulate your affected areas of skin.
Practically speaking though, unless the disease has
- already stabilised and
- is affecting only very small areas of the skin,
the process of repigmentation can be very slow. [6]
In the majority of cases that I have experienced, patients may have minimal repigmentation even after many years.
If you would like to achieve more rapid repigmentation, there are certain treatments available. I will elaborate on this later in this article.
Can vitiligo be prevented?

I would say a better way to think of this question is: “How can I avoid triggers for vitiligo?”.
Identifying your own specific triggers for vitiligo and avoiding them can help somewhat to prevent further triggers for the condition. For example, you can avoid excessive sun exposure and use sun protection as needed.

The internet is filled with multiple sources claiming the benefit of certain foods or specific diets for the treatment of vitiligo. However, we must bear in mind that dietary research is extremely difficult to conduct reliably. Just looking back for the past couple of decades, dietary advice has flip-flopped on things like sugar, fats, red meat, and even coffee.
Realistically speaking, I advocate a healthy and balanced diet for all my patients when necessary, taking care to ensure they eat at least the recommended daily amounts of fresh fruit and vegetables. If possible, do eat a variety of colours of fruits and vegetables to get a good spread of trace elements and minerals in your diet. [7]
How is vitiligo diagnosed?
The diagnosis of vitiligo is based on the clinical examination of your skin. A thorough top-to-toe examination may often reveal additional areas of pigment loss which patients are unaware of. Some examples of areas which patients may be unaware of include the back, the scalp, and the genitals.
Beyond examination under normal lighting, examination with a Wood’s lamp lets your doctor identify depigmented regions of skin. A Wood’s lamp can also identify new areas of partial pigment loss which may not be apparent under normal lighting. The Wood’s lamp emits UV light which causes depigmented skin to fluoresce white. The affected patches will appear to glow under the lamp.
This examination, paired with the history of progression of the condition, allows your doctor to differentiate between vitiligo and other similar conditions. Do tell your doctor if you have had recent infections, preceding traumas, allergies, stressors, or changes in skin exposure, including new soaps or detergents. This is relevant information for him or her to take into account for your diagnosis. [8]
I have had some patients who suspected they had vitiligo when it was not the case. Some examples of similar conditions would be:
- Postinflammatory hypopigmentation
- Chemically induced depigmentation
- Pityriasis alba
- Tinea versicolor
- Idiopathic guttate hypomelanosis
Can vitiligo be cured?
There is no cure for vitiligo. People with a tendency to form vitiligo will be at risk of having their condition recur or flare.
However, the progress of vitiligo can be slowed down and your skin can regain its pigment, either by UVB light treatment, or on its own.
How is vitiligo treated in Singapore?
There is no one-size-fits-all treatment for vitiligo, but rather, there are a number of different treatments available. More often than not, early diagnosis and treatment lead to better outcomes.
Timely treatment can help to prevent or limit the extent of depigmentation of your skin. This also helps curtail the physical and emotional or psychological effects of vitiligo.
Below, I will cover a few main treatment modalities which are commonly available in Singapore.
With so many treatment options available, it is important to understand a bit more before you decide which ones to proceed with.
Beyond the choice of therapy, your treatment outcomes are heavily dependent on how consistent you are with treatment (e.g. applying creams daily, not missing sessions of phototherapy) and how our comply with therapy (e.g. persisting with therapy for the stipulated duration, and not giving up halfway). The most common thing that I hear from all my patients who have previously failed therapy is that they got lazy, or gave up on treatment prematurely.
Ultimately, your treatment should be tailored to your individual needs. This will factor in things such as the extent of your depigmentation, your main areas of concern (e.g. patches on the face), and schedule, just to name a few.
Topical/oral corticosteroids
Topical corticosteroids are skin creams or lotions that contain steroids and are often the first treatment offered for patients with vitiligo. When applied, it works by suppressing the inflammatory response of your skin. It is more often used if you have limited areas of vitiligo affecting less than 10% of the body.
The main concern with corticosteroids are the side effects that come with prolonged usage. Some of these are localised skin atrophy, skin thinning, easy bruising, visible or enlarged blood vessels, and easy breaking of skin. A few of these side effects can go on to affect the whole body.
However, in some patients with rapidly developing depigmentation of the skin over large areas of the body, there may be a role for oral corticosteroids instead. This allows the stabilising effects of corticosteroids to be delivered to your skin all at once.
Some areas of the body are not so suited for topical corticosteroids. This brings me to the next class of medicines. [9]
Topical calcineurin inhibitors

For certain patients, your doctor may prescribe topical calcineurin inhibitors such as tacrolimus (more commonly known by its brand name Protopic). This is a non-steroidal cream and can be applied over the areas around the eyes safely. It avoids the common side effects associated with steroids -- the main ones being a slight burning sensation which tends to resolve within a few days with use. [10]
Topical Vitamin D analogues

A vitamin D analogue refers to synthetic vitamin D that is applied to your skin. It works to inhibit some immune cell activity and promote pigment cell maturation and growth.
Besides vitiligo, vitamin D analogues can also be used to treat osteoporosis and psoriasis. Examples of vitamin D analogues include calcipotriol and tacalcitol. These are most often used in combination with phototherapy. [11]
Phototherapy

Beyond creams, the next most commonly used technique for purposes of vitiligo is phototherapy. Phototherapy refers to exposure of your skin to ultraviolet A (UVA) or ultraviolet B (UVB) light from a lamp. This light stimulates the pigment-producing cells in your skin to multiply.
In the past, some patients were asked to apply or consume photosensitising medicines before exposing their skin to the sun. Over time, the development of specific machines allowed for controlled dosing of UV light to the skin.
Currently, the main form of phototherapy used today for purposes of vitiligo is narrow-band UVB phototherapy. This uses a specific wavelength of UV light and not the full spectrum in order to deliver better rates of repigmentation of your skin.
This treatment is generally well-tolerated, even among children and pregnant ladies. The main concerns with narrow-band UVB phototherapy are that of sunburn and possible reactivation of herpes simplex in patients with preexisting disease. [12]
Phototherapy is often offered in conjunction with the above mentioned topical creams in order to obtain better overall results. Response to phototherapy will depend on a few key factors, which include the duration of your vitiligo, areas of your skin affected, and your own sensitivity to light.
The main stumbling block for patients considering phototherapy is the time commitment involved. For a start, patients are most commonly recommended a treatment frequency of two to three times a week. The majority of working adults or school children are unable to achieve the recommended treatment frequency, due to a mismatch between their free times and times when a phototherapy unit is open and available for their use.
I often counsel my patients that patience and consistency are the keys to successful vitiligo treatment. While generally, patients may start to see some signs of repigmentation anywhere within 10 to 30 sessions, full repigmentation may take even longer.
Grafting
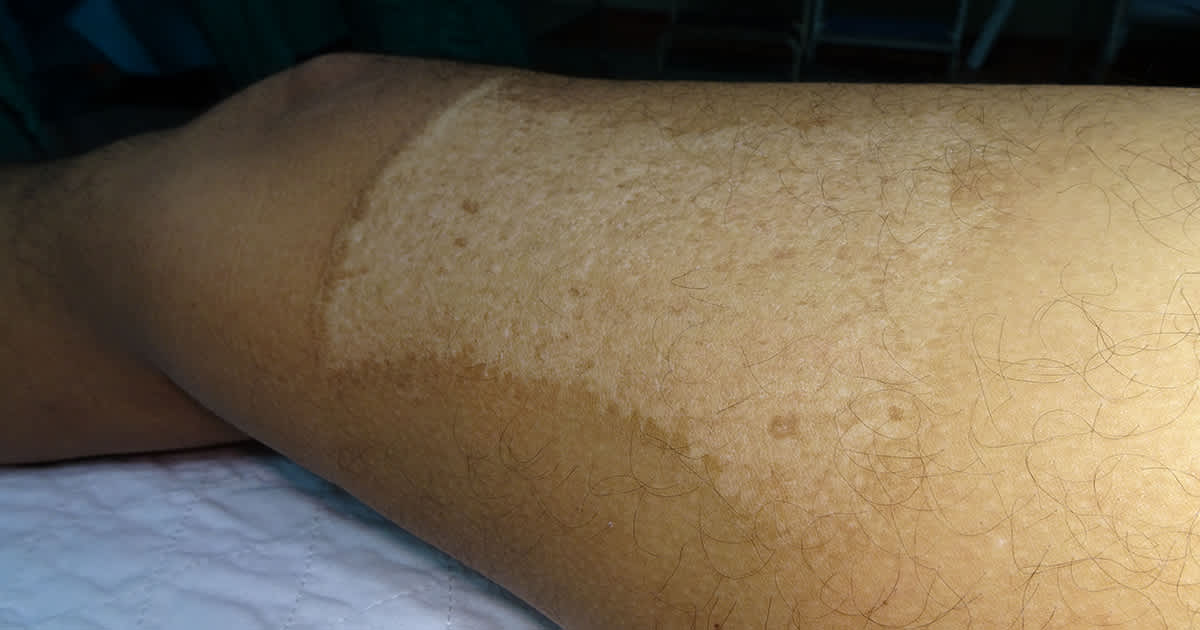
The hands and feet, and in particular, the fingers and toes, are known to generally have a poorer response to phototherapy and topical treatments. In these cases, there is sometimes an option of some procedures to help increase the response rate, such as skin grafting.
There are many different grafting techniques which have been described in medical studies. Their general principle is that healthy pigment from an unaffected skin area can be transferred over to an area with no pigment. The transferred pigment cells then act as a point from which future pigment cells can multiply and grow to cover the depigmented regions.
For the most part, doctors only consider procedures mentioned above if your condition has been stable for 6-12 months. Performing these procedures in early or actively spreading vitiligo may result in a worsening of the condition. [13]
Other treatments

There are many more available treatments which are out there, some of which are early and experimental and some of which are slightly less evidence-based. I have heard a number of different folk remedies described to me in the clinic, all of which have had disappointing results for my patients. If you are considering or are unsure about any given treatment for vitiligo, my recommendation would be to find a doctor whom you are comfortable with and to clarify any questions with him or her before starting on anything new.
Most treatments advertised as natural cures for vitiligo are relatively harmless, and others may be a waste of time and effort at worst. However, I have also heard of more drastic and traumatic alternative therapies for the treatment of vitiligo which have left long-lasting scars on my patients.
Contrary to the popularly held belief that vitiligo cannot be treated or is a life sentence, even among some members of the medical community, there are actually many available options. In fact, the field of study is growing, and more and more research is being conducted to find new and alternative methods and medicines to better address the needs of patients.
But does Vitiligo treatment really work? An overview of recent research results.
Recent research on vitiligo treatment from Singapore within the last ten years has found that:
Cellular grafting achieved 65% or higher amounts of repigmentation within six months after treatment among patients with stable vitiligo. These results remained constant after one year. [14]
Another study found that 83% of patients who had undergone noncultured cellular grafting for vitiligo achieved good to excellent repigmentation at the 60-month mark. [15]
Phototherapy is effective and safe for treating vitiligo in Asian children, including Indian children with darker skin tones. Patients with generalised vitiligo responded better to phototherapy treatment than patients with segmental vitiligo. Side effects reported were mild and including itching, scaling, pain, erythema, sunburn, blisters, and phototoxicity. [16]
A National University of Singapore study also found that providing a suitable health consultation helps patients living with vitiligo to maintain their psychological health and alleviate symptoms of depression. [17]
When should I seek treatment for vitiligo?

If you suspect that you or a loved one may have vitiligo, it is best to seek a doctor’s consultation as early as possible. There are a number of different conditions which can appear similar to vitiligo. Besides ruling out other possible medical conditions, early management of vitiligo can help to slow its progress and deliver good outcomes.
This does not mean that patients who have had long-standing vitiligo cannot be treated. The same treatments are still available to them, though their individual response to therapy may be slightly different.
Of course, there are individuals who choose not to seek treatment for their vitiligo and instead embrace their changes in skin colour. Self-esteem is understandably a big reason people seek treatment for any skin conditions. I admire and commend patients who are able to live with this very visible skin condition confidently.
It is heartening to me when I hear from patients that their families and friends accept them for who they are, rather than how they look due to their condition. However, when it comes to the workplace, customer-facing staff, sales personnel, or businesspeople often are keen to address their vitiligo so as to minimise any impact on their career.
Where can I get treatment for vitiligo in Singapore?
Medical doctors and dermatologists provide vitiligo treatment in Singapore. As every patient with vitiligo is unique, a treatment plan should be customised for your needs.
Check where you will be receiving treatment (if it will be in the same facility as the consultation clinic), and if the treatment sequence and time slots fit your schedule. This will help with what doctors call “compliance” with treatment - how closely you are able to stick to your treatment plan, that is needed for the best possible results for your condition.
The main reason for sub-optimal treatment outcomes tends to arise from:
- premature ending of treatment
- poor adherence to treatment
Treatment of vitiligo, like any other chronic condition, requires both commitment and patience to see it through. Finding a doctor whom you are comfortable with and can help you to understand the treatment process and what it involves is crucial.
Also read: 8 Dermatologist Clinics in Singapore for Your Skin Concerns (2020)
What are the costs of vitiligo treatment in Singapore?
Costs for vitiligo treatment vary in Singapore. Here is an indicative but non-exhaustive range of how much different aspects of vitiligo treatment may cost. Do note that this does not take account of any adjustments in dosage or total duration of treatment.
Costs for each aspect of treatment vary based on several factors, some of which are noted in the rightmost column. Do feel free to send a treatment quote enquiry to find more personalised information on treatment costs.
Treatment or medication
Cost (SGD)
Frequency
Notes
Topical corticosteroids
$ 100 onwards
Applied to effected areas twice a day
Varies depending on total surface area affected
Topical alcineruin inhibitors
$ 100 onwards
Oral corticosteroids
$ 30 - 40
Most often taken 2 days a week for 12 weeks
Phototherapy
$ 50 onwards
Recommended as 2 - 3 times a week, min 24 hours apart
At a minimum, 10 to 30 sessions are needed. More sessions are needed for patients with existing vitiligo or for whom repigmentation is slower.
Excimer Treatment
$ 100 onwards
Performed to targeted areas, more suitable for certain areas like the face.
Procedures
Ranges widely depending on total area affected. Only suggested for specific patients with stable conditions for 6-12 months.
Can I get subsidies for vitiligo treatment?

In Singapore, vitiligo treatments are claimable from Medisave under certain conditions.
For patients above the age of 60 in Singapore, treatments and medications for vitiligo at polyclinics, specialist outpatient clinics, and CHAS general practitioner clinics are claimable under Flexi-Medisave.
Patients are not able to make claims under MediSave500 as vitiligo is not classified as a Chronic Disease Management Programme condition in Singapore.
Inpatient medical treatments such as skin grafting surgery are claimable in Singapore, as per all other inpatient medical treatments. [18]
How can I find the best vitiligo doctor for treatment?
There is no such thing as a “best doctor” but the most appropriate doctor for each individual. When looking for a doctor, do consider any of the following:
The philosophy, bedside manner, and approach of the doctor
Find a doctor who makes you feel comfortable and whose perspective on vitiligo treatment you can agree with. In addition, it is important to find a doctor who understands not only your skin condition but also the associated psychological conditions vitiligo patients may go through. Only vitiligo patients will know this, but it is a deeply personal and sometimes harrowing experience to have to recount.
As with any skin condition, patients with vitiligo may experience personal embarrassment and even depression. According to a study in Singapore, 16.2% of patients with vitiligo had depression, based on the Epidemiologic Studies Depression Scale. [19]
Location of clinic
Vitiligo treatment takes patience and can stretch into months of regular clinic visits. That’s why a clinic that is accessible to your work, school, or residence will be easier to fit into your regular schedule of follow-ups and treatments.
Medical team
Does the doctor work with other experienced nursing staff? They will be part of the team assisting in your care.
Facilities
If you are undergoing phototherapy, it is important to understand more about your phototherapy device. Phototherapy is a broad umbrella term which takes many forms, some of which are more effective for the treatment of vitiligo than others. Knowing your UVA from your UVB and more importantly, what devices are being used in the clinic means you will know exactly what to expect from treatment.
How many cases of vitiligo the doctor has treated
A doctor who has training and experience working with patients with vitiligo has a wider knowledge of the condition and its side effects and treatments. Do ask your doctor about the previous cases he has treated, noting that every patient is different and treatments work differently on each individual.
A holistic and interdisciplinary approach is useful for the treatment of any long-lasting health conditions. Find a doctor who does not just treat your skin but who can provide advice and referrals for other conditions you have.
What should I ask my vitiligo doctor in the first consultation?

When I meet patients for the first time, there are key aspects of their history which I need to know in order to formulate an effective treatment plan. Their medical history and associated conditions (such as autoimmune history, family history of vitiligo) are chief among them. Beyond that, I find that their occupational history (and associated occupational hazards/exposure) as well as history of development of their condition allows me to better understand how best to begin treating them. Standout aspects such as preceding trauma, sun injury, abnormal periods of stress arising from either the workplace or from home, all of these can give clues as how best to approach.
Tell your doctor when you started noticing any vitiligo patches, and if you have noticed any growth in response to certain periods in your life. Photo documentation of affected areas allows for a clear understanding of the changing skin condition.
I have found it best to help patients who come with their histories all in order, including any previous treatments, orthodox or otherwise.

I hope this article has helped to shed light on this commonly misunderstood condition, and given you more information on what to discuss with your doctor during a skin consultation about vitiligo-related concerns.
Remember that vitiligo is only part of the picture of your overall health, which should be managed not just by your medical team but also by yourself in a holistic manner. It is good to keep up an active social schedule, and set goals in life that motivate you to help not just yourself but also others. This will help make your life more than just this skin condition.
Dr David Tan is an experienced Singapore's Ministry of Health accredited doctor. Besides treating general skin conditions, his areas of interest include managing vitiligo, skin laser treatments and aesthetics dermatology. Dr Tan graduated with an MBBS from Australia. Following that he has gained a Diploma in Clinical Dermatology and is certified in Ablative and Fractional Lasers in Singapore. On top of all that, Dr Tan is also trained in Internal Medicine in Singapore and USA.
Would you like to ask any related questions about vitiligo?
You can Ask A Doctor right away, or view the complete list of Human Sessions.












