Endometriosis is one of the most common conditions women suffer from. Globally, it affects 22% of all women [1].
It is one of the main causes of infertility in Singaporean women. This is also the case in other countries. Research has shown that 50% of all infertile women have the condition [2].
I am writing this to help you understand more about endometriosis. I will talk about its symptoms, treatments, and also management. Read on to find out more!
What is endometriosis?
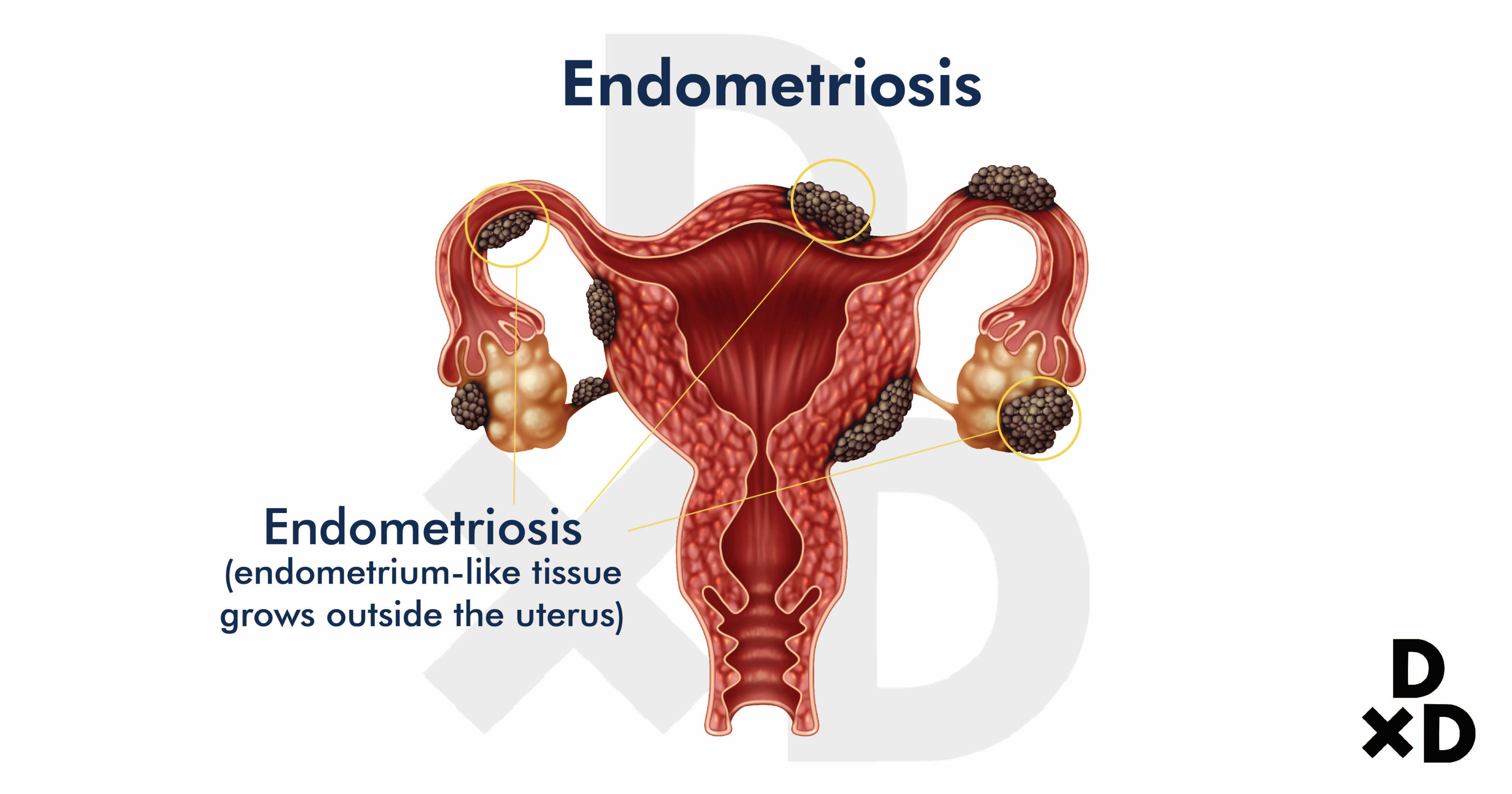
Endometriosis is a condition where an endometrium-like tissue grows outside the uterus.
The endometrium is the layer that lines the walls of the uterus. This is the layer that breaks down and is shed each month when you have your period.
The abnormal growth is most commonly found around the pelvis, especially in the:
- Ovaries
- Fallopian tubes
- The surface of the uterus
- Pouch of Douglas (the space behind the uterus)
- Bowel
- Bladder and ureters
- Rectum
Very rarely, they can also be found in the lungs, brain, and skin [3].
They can be classified into 4 stages:
- Minimal (Stage 1)
- Mild (Stage 2)
- Moderate (Stage 3)
- Severe (Stage 4)
Note that for endometriosis, the stages are not related to the amount of pain or discomfort felt by the patients. There are different ways the condition may appear and cause a problem. In some cases, someone with stage 1 can feel more pain than a patient with stage 4 endometriosis.
This classification is based on the: [4]
- Location
- Amount
- Depth
- Size
They can cause chronic pain
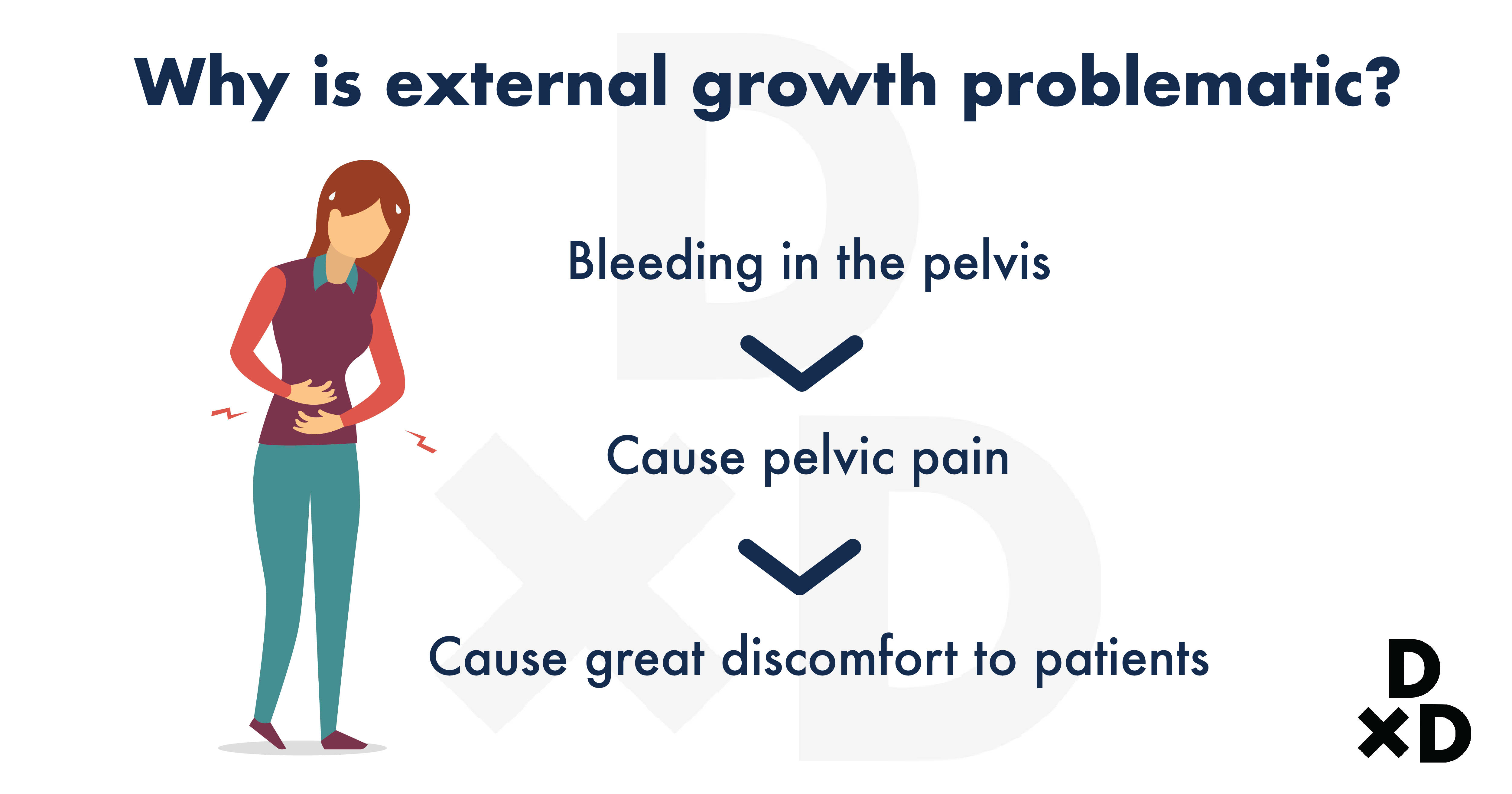
The tissue is abnormal in how they react to hormonal changes during your period. They can break down and cause bleeding in the pelvis. This pool of blood causes inflammation and build-up of scar tissue called adhesion. They can bind organs together and cause pelvic pain.
When these tissues appear in the ovaries, they can also form cysts [4].
Endometriosis is non-cancerous. They also do not spread by contact. That said, they can still cause great discomfort to affected patients. The condition has been found in many cases of chronic pelvic pain [1].
Who are at risk of endometriosis?
Though we do not know the exact cause of endometriosis, we know that it is related to changing hormone levels. This is why endometriosis is more common in women of child-bearing age [1]. This refers to women in their 20s – 40s.
That said, endometriosis can be found in any female who has their first menstruation. I have seen patients across a range of ages suffering the condition. Though uncommon, I have also met teens with the condition.
Not a lot of teens are diagnosed with the condition. This is because the symptoms are very similar to normal menstruation [5]. If you constantly feel pain during your period it would best to visit a doctor! They may be normal characteristics but it is a good idea to find out the actual cause.
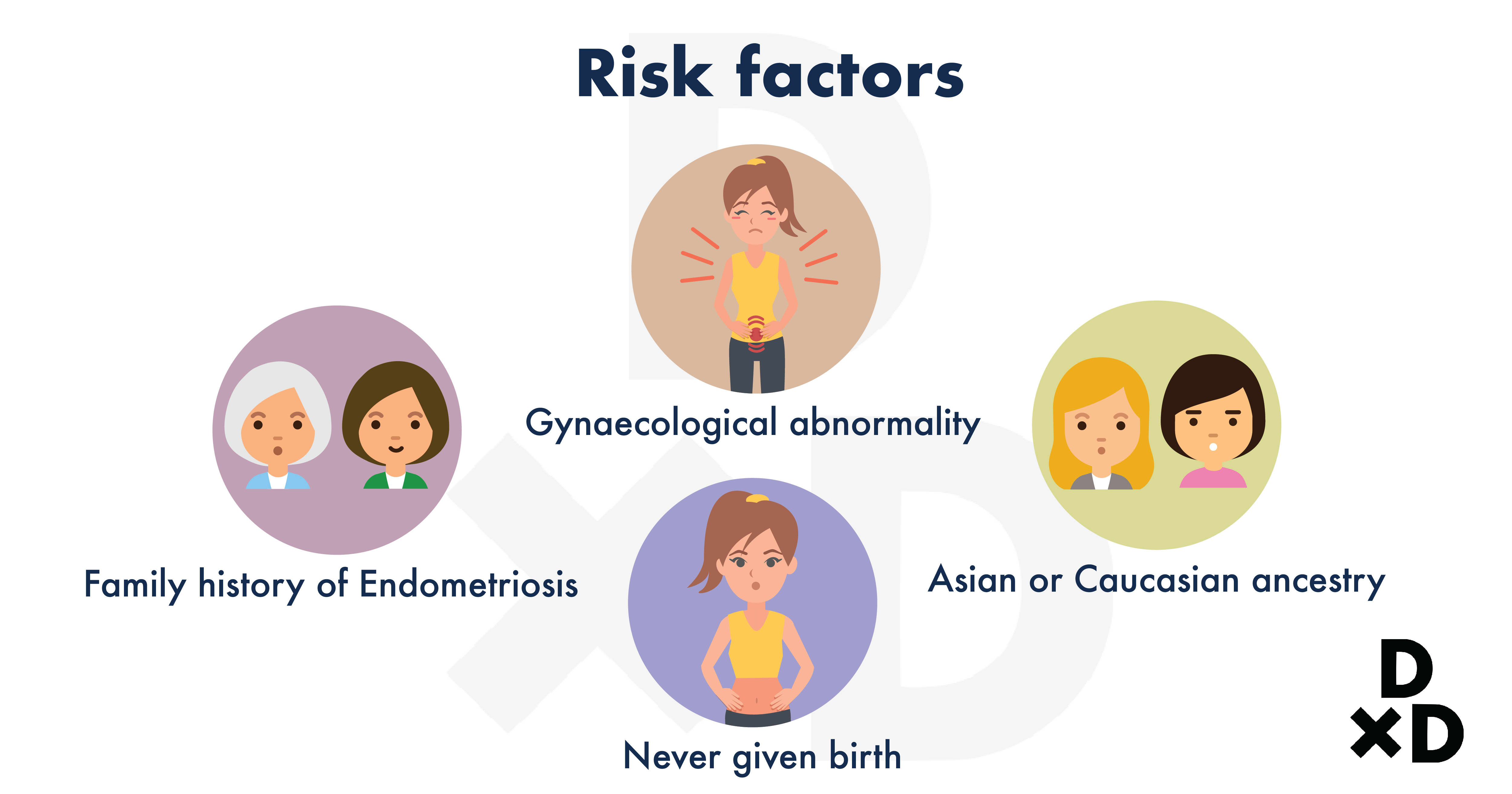
You might have a higher chance of developing the condition if you have: [6]
- Never given birth
- Family members who have had the condition
- Gynaecological abnormality (blocked vagina, deformed uterus, etc.)
- Asian [7] or Caucasian [8] ancestry
What are the symptoms of endometriosis?
The experience can differ between each person. Common symptoms are: [9]
- Heavy, painful, and/or irregular periods
- Pain during sex
- Constant pelvic pain
- Problems in the bowel and urinary functions
- Blood in the urine (haematuria) and stool during monthly periods
- Infertility
Often times, the pain may also affect women’s mental well-being [10].
There might also be blood in the lungs when you have your periods if abnormal tissues are found there. Though rare, some women may also cough blood because of this.
Remember, this might not be your case! Endometriosis may show other symptoms and at times, they can also present no symptoms at all.
You might notice that the symptoms are actually very common. They are quite similar to diseases such as appendicitis and cysts. This is most likely why the condition is often undiagnosed.
If you experience any symptoms, it would be best to visit your doctor as soon as possible!
How is endometriosis diagnosed in Singapore?
The first step is a consultation with your doctor. If your doctor suspects the condition, they may recommend one of the following tests: [2]
- Pelvic (transvaginal) ultrasound scan
- Detailed vaginal and rectal examination
- CT scan or Magnetic Resonance Imaging (MRI)
- Blood test (Ca125)
- Laparoscopy
Above is just a list of diagnostic tests commonly used in Singapore. Depending on your condition, doctors may use either one or a combination of the tests. To know exactly which ones you need, do consult your doctor!
How is Infertility linked with Endometriosis?
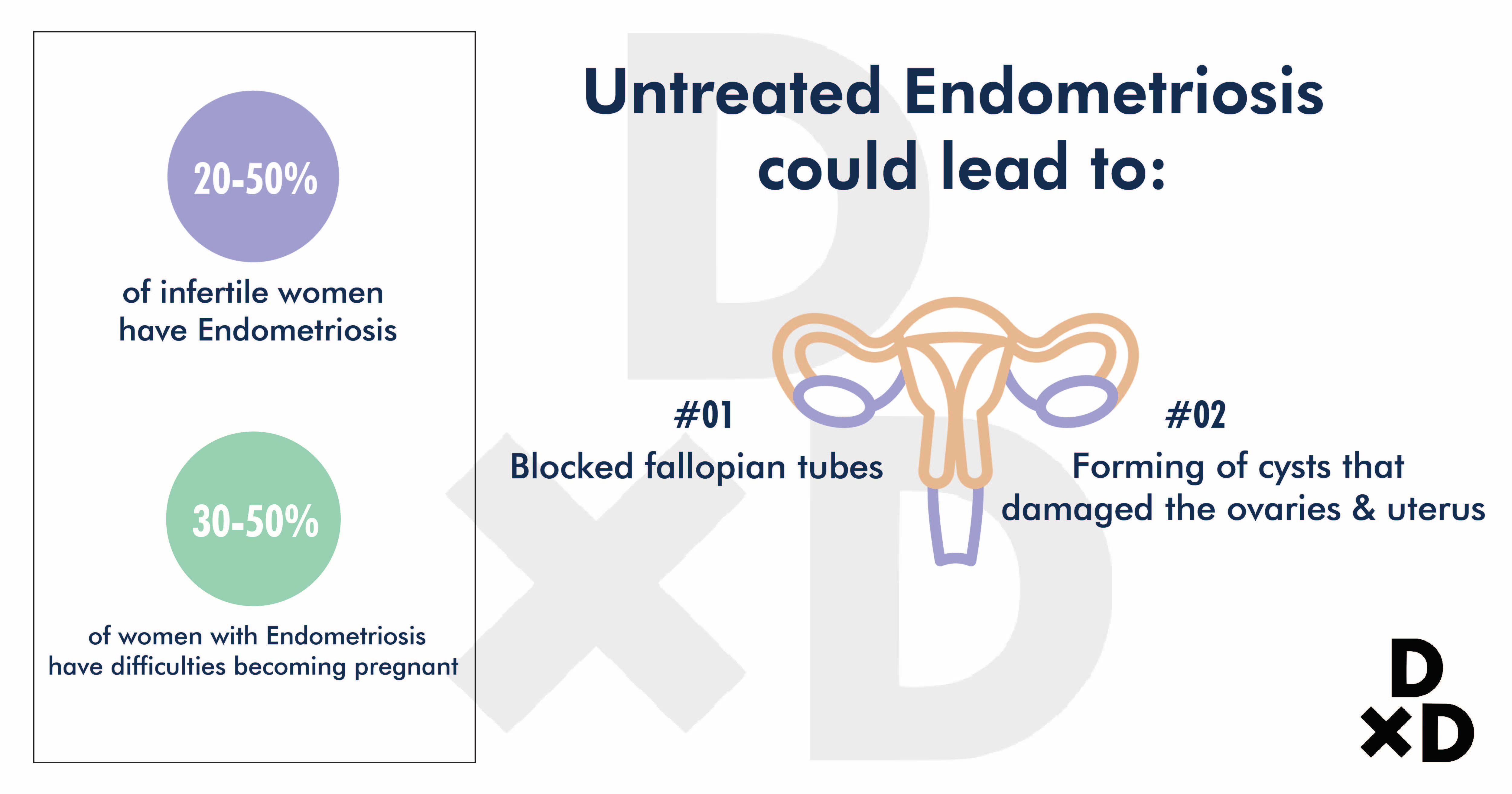
Endometriosis is found in 20-50% of all infertile women. A study has also found that 30-50% of women with the condition have difficulties conceiving [10]. This shows a strong relation between the two conditions.
Infertility can be caused by a lot of different factors. It could be in the male, the female, or in both. As a general guide, you should seek a doctor if you are unable to conceive after:
- 1 year of active intercourse for women under 35 years old
- 6 months of active intercourse for women above 35 years old
Endometriosis should not be left untreated. This is because its symptoms tend to worsen over time. On top of that, endometriosis is also known to have a high recurrence rate.
The build-up of endometrium-like tissue can:
- Block fallopian tubes
- Form cysts that damage the ovaries and uterus
This is a huge concern as scarring in the fallopian tubes accounts for 30% of women infertility cases. Ovulation problems are also found in 20% of the cases [11]. The link between the two conditions has been known for some time. That said, we still do not understand the exact way they are connected.
Surgical treatments have been found to increase the chances of pregnancy. Your doctor may also give you oral medications to prevent recurrences. In some cases, you might also need hormonal therapies. That said, they are not able to cure the underlying disease.
Related: How does endometriosis affect IVF?
How does pregnancy & breastfeeding affect Endometriosis?

For some women, being pregnant can help manage the symptoms of endometriosis. This is because pregnancy suppresses the hormones that trigger the menstrual cycle. It is important to note that this does not cure the disease. Symptoms may or may not recur after the birth of the child.
If you have endometriosis, it is best not to delay having children. This is because the symptoms tend to worsen over time. The longer you wait, the harder it may be for you to conceive.
If you have problems conceiving, you might have to get surgical treatments. They have been found to significantly improve live birth rates [12]. You should note that pregnancy rates are highest within the first year after the surgery. As time goes, symptoms tend to recur.
Does breastfeeding help manage endometriosis?
Most women can delay the recurrence of symptoms by breastfeeding. However, this is only true if you breastfeed frequent enough to stop your menstrual cycle.
A study found that women who breastfed were at a significantly lower risk of endometriosis compared to those who do not. This is true for 5 years after giving birth [13].
The study also found that the risk decreases even more if you breastfeed for a longer-term. This is because the longer you breastfeed, the longer you might stop your menstrual cycle.
What are non-surgical treatments for endometriosis in Singapore?
As of now, there is no cure for endometriosis. That said, there are medications and therapies you can take to help manage the symptoms.
Treatments are aimed to:
- Relief pain
- Prevent recurrences
- Suppress the development of endometriosis tissue
- Treat infertility
The first line of treatment is should be non-surgical [14]. They come in the form of:
Pain Medication
Anti-inflammatory drugs (NSAIDs) can help with menstrual cramps. They are also used to help manage chronic pelvic pain. If you are taking over-the-counter painkillers, remember to declare them when you consult a doctor.
Hormonal Therapies
They help relieve pain by holding off the hormones related to the menstrual cycle. They can reduce your menstrual blood flow by limiting the thickness of the endometrium. On top of that, they also decrease the growth of abnormal tissues.
A few examples:
- Combine oral contraception pill (Yaz, Yasmin)
- Intrauterine contraception (Mirena)
- Depot progesterone injections (Depo-Provera)
- Oral progesterone (Visanne)
- Gonadotropin-releasing hormone (GnRH) agonists (Lucrin, Zoladex)
- Danazol
Though these can effectively relieve pain, they also limit fertility. If you are planning to have children, you might have to find other alternatives. You should always consult your doctor to find which one is most suitable for you!
How do surgical treatments to improve fertility?
Surgical treatments should only be taken if all other treatments have failed. You might also need surgery to treat:
- Infertility
- Severe chronic pain
- Enlarged cyst
Surgery can remove:
- Lesions
- Ovarian Cysts
- Scar tissue (adhesions)
- Visibile abnormal tissue
On top of that, they have been found to improve fertility.
Most women with no fertility problems have an 84% chance of getting pregnant within 1 year of active sex. For those with endometriosis, the chance decreases to 30-50% [10]. This may vary between patients. It really depends on the severity and location of the abnormal tissue.
A study found that there is a significant increase in the chances of pregnancy: [15]
- For patients with mild cases, the chances improve to:
- 81% with laparoscopy
- 84% with laparotomy
- For patients with moderate or severe cases, the chances improve to:
- 54-66% with laparoscopy
- 36-45% with laparotomy
This is not accounting for other factors such as sperm and egg quality, and whether or not the women ovulate in the first place.
These days, laparoscopic (key-hole) surgery is much more common. This is because they are:
- Less invasive
- Needs only a short time for recovery
In any case, always consult your doctor! The most effective treatment is one that is specialised to you.
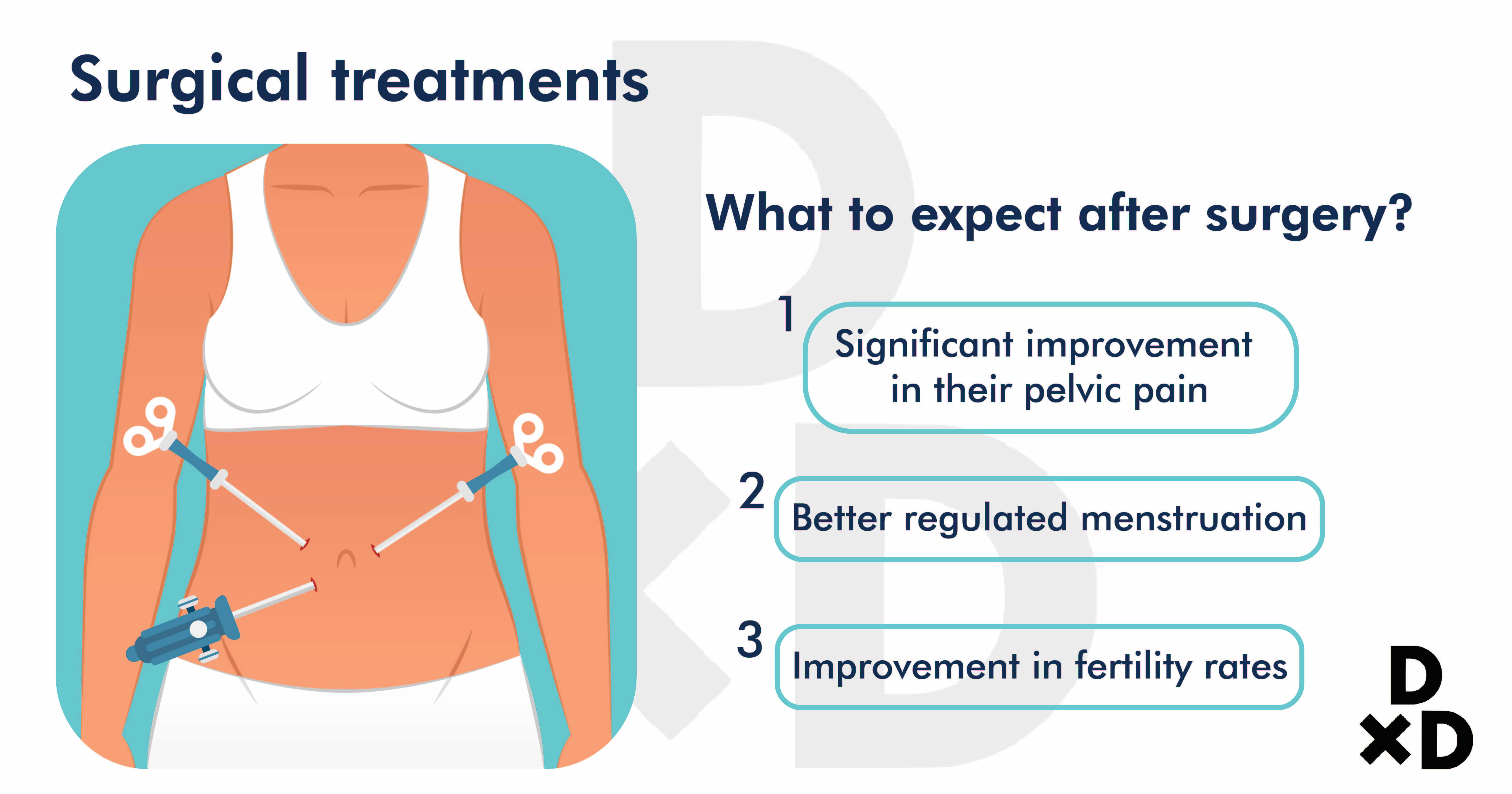
What to expect after the surgery?
Most women report:
- Less pelvic pain
- More regular periods
- Better fertility rates
What are the risk factors?
The procedure is safe. In most cases, there should be no complications. That said, there are still some high-risk factors. Though rare, this includes bowel, bladder, ureteric, and blood vessel injury.
The most common side-effect is the recurrence of symptoms. That said, this risk should remain quite low with hormonal treatments after the surgery.
Other common risk factors include:
- Tender skin
- Wound infection
but in most cases, they resolve within a few days.
If you feel any discomfort after the surgery, it would be best to contact your doctor immediately. This is also true if you still feel constant pain.
Is there a definitive surgical treatment for Endometriosis?
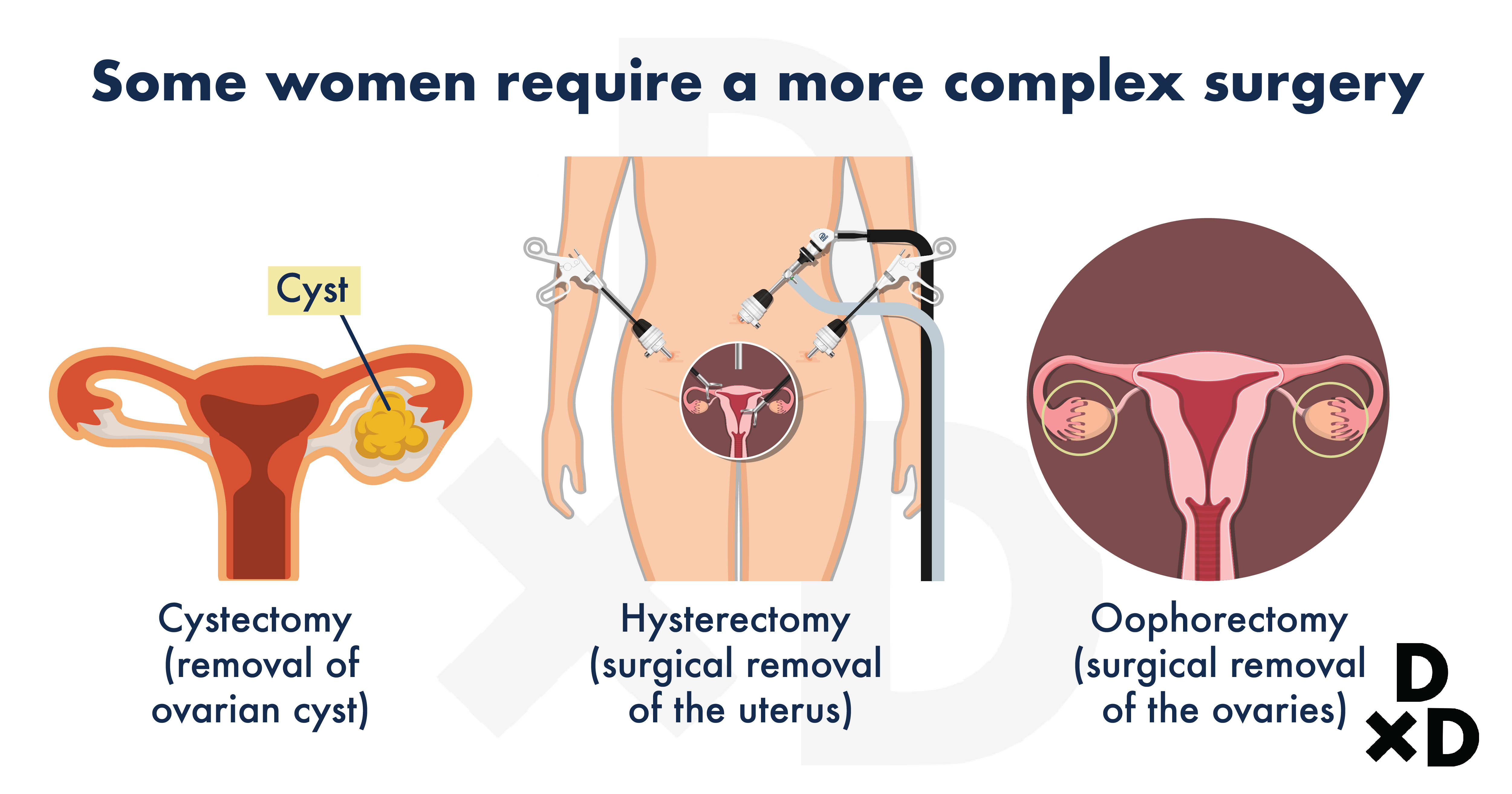
For some women, the pain might be so severe that they require more complex surgeries. These might include:
- Cystectomy (removal of ovarian cyst)
- Hysterectomy (surgical removal of the uterus)
- Oophorectomy (surgical removal of the ovaries)
- Or both hysterectomy and oophorectomy
A study has shown that those who only had a hysterectomy have a higher risk of pain recurrence as compared to women who had both procedures. They also have a higher chance of needing a second surgery [16].
It is important to note that when the ovaries are removed, women would no longer be able to conceive. They would also experience surgical menopause. The symptoms will start within a few days of the surgery.
On top of that, there are also other risks, both physical and psychological. You can find out more about that in my hysterectomy article.
Also read: The Ultimate Guide to Hysterectomy in Singapore (2021)
If you are searching for treatment, it is best to consult a doctor. This is because cases vary between patients. It is important that you get a treatment that is specialized to you. Doctors can figure out which treatments are best for you through a detailed consultation and health screening!
Bottom line is, always do research to find out about all the available treatments! You should discuss all the pros and cons of a certain treatment with your doctor before giving consent.
How can I management my mental well-being?

Even with oral medication, surgeries, and therapies, it could be quite devastating to know that the condition has no real cure. That outlook and the chronic pain it caused can really impact a woman’s mental well-being.
Research has shown that women report: [17]
- Anxiety
- Depression
- Loss of focus and concentration
- Limitations in social life
- Overall poor quality of life
Some young girls with severe symptoms may also have to take time off school or sports to manage the condition. This is why the condition can be a huge hindrance.
It is important to note that your psychological stress might trigger more pain. For that reason, you should also take care of your mental well-being on top of medical treatments! They are as important as managing your physical pain.
If you need help you can always consult your doctor. Some clinics even have professional mental health services for patients. On top of that, there are support groups in Singapore that can help you deal with the condition.
Also read this guide on Gynaecological conditions in Singapore
I wrote this article to help you understand more about endometriosis. It is a common gynaecological condition and its treatment can be quite complex.
I certainly help this helps your research! If you have any symptoms or discomfort around your pelvic area, it is best to consult a doctor as soon as possible. Be it endometriosis or under gynaecological conditions, it is best to diagnose and treat them early!
Dr Christopher Ng is a gynaecologist with GynaeMD Women's & Rejuvenation Clinic. He is accredited to perform Level 3 laparoscopic (minimally invasive) surgeries on top of general gynaecology surgeries. He also performs surgery for urinary incontinence and uterovaginal prolapse.
Read more of Dr Christopher Ng's QnA here.
Would you like to ask any related health questions?
You can Ask A Doctor right away, or request for treatment quotes from doctors.