This guide explains all you need to know about getting a colonoscopy in Singapore, including who should undergo a colonoscopy and why, the preparation required, the actual process as well as the cost incurred and current trends in Singapore.
I have written this article from my experience as a doctor (the first female colorectal surgeon at the Singapore General Hospital!) to explain the importance of a colonoscopy. I also hope to clear any doubts you may have and alleviate any fear of the procedure in an attempt to promote healthier colon health for all.
We have other articles on appendicitis and food poisoning on Human!
Colonoscopy: What is it?
For starters, what is a colonoscopy? Well, a colonoscopy is a medical procedure that involves inserting a long, flexible tube called a colonoscope through the anus of the patient.
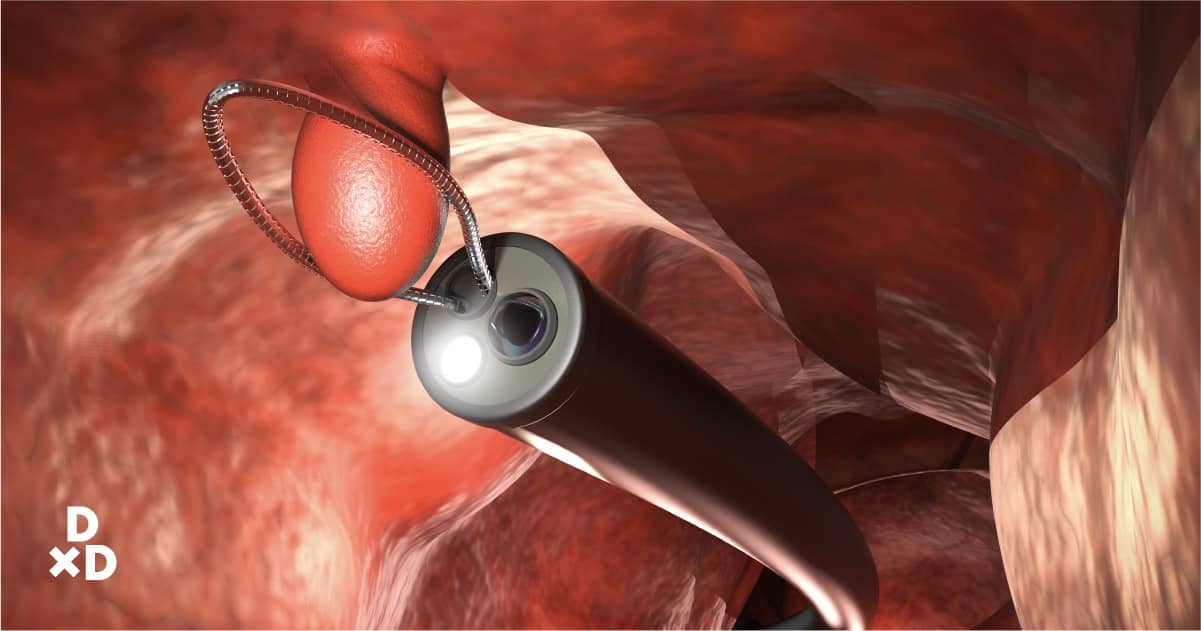
A tiny camera at the tip of the colonoscope allows your doctor to examine the inside of the colon(large intestine) and the rectum to detect any abnormalities. Sort of like a gastroscopy, but from the rear end! [1]
I use this to screen for colon cancer in my patients because it also allows the detection of pre-cancerous polyps or adenomas. Biopsies are performed if suspicious-looking growths are seen during the colonoscopy to determine the nature of the condition. If polyps are found, removal of the polyps is performed at the same time.
Why is a Colonoscopy so important in Singapore?
Colorectal cancer is the number one most common cancer diagnosed in the Singapore resident population, affecting close to 2000 individuals yearly.
It is the most common cancer amongst men and is second only to breast cancer in women. Consequently, colorectal cancer is amongst the top 3 leading causes of cancer deaths in both men and women in Singapore [2].
Worldwide, colorectal cancer incidence and mortality in patients younger than 50 years old are increasing. Furthermore, our local statistics indicate that up to 1 in 5 Singaporeans who are diagnosed with colorectal cancer are under 55 years old.
The American Cancer Society recommends that people at average risk of colorectal cancer start screening at 45 years of age. This is as opposed to the previously recommended age of 50 due to the rising worldwide incidence of colorectal cancer.
In Singapore, the Ministry of Health still recommends screening for an average risk individual to begin at age 50. However, individuals with a family history of colorectal cancer may need to start screening at an earlier age.
For example, I suggest my patients to start screening at age 40 or 10 years prior to the youngest case in the family (whichever is younger) if there is one 1st degree relative with colorectal cancer below the age of 60.
Colorectal cancer screening has been proven in many research studies to decrease the incidence of colorectal cancer. This is achieved mainly by the detection and removal of precancerous adenomatous polyps during colonoscopy, effectively preventing the progression of the polyps to cancer.
Costs of Colonoscopies in Singapore
There are different factors to consider when it comes to colonoscopies which lead to different costs:
Public hospitals with subsidy
Restructured Hospitals
Private hospitals
$300-$830
$1,100-$2,500
$1,800-$2,600
Prices are easily obtainable when you call or send in an enquiry to the centres where you are interested in having your colonoscopy.
Note that the price quoted can increase if a biopsy or polypectomy is performed.
The base cost of a colonoscopy in private hospitals is $1,800 - $2,600. The cost at a restructured hospital ranges from $1,100 - $2,500, depending on whether you are eligible for subsidies [5].
If biopsies, polyp removal and/or histological analyses are required, additional cost will be incurred due to the use of additional equipment and tests required.
Performed as a day surgery procedure, Singaporeans and permanent residents can use up to $1,250 from their Medisave to pay for the procedure [5].
Who should get a Colonoscopy in Singapore?
In accordance with the recommendation from the American Cancer Society, individuals with an average risk of colorectal cancer should be screened for colorectal cancer from 45 years of age.
In Singapore, we commence screening:
- When you are 50 years old
- Before you are 50 years old if you have an increased risk (e.g. a family history of colorectal cancer or related cancers).
Do note that these guidelines only apply if you do not have symptoms.
However, there are a variety of symptoms that may warrant colonoscopy earlier. These symptoms include:
- change in bowel habits
- blood and or mucus in the stools
- unexplained weight loss and/or appetite
- abdominal bloating or pain
In addition, as mentioned above, individuals with a family history of colorectal cancer may need to start screening at an earlier age.
A colonoscopy is just a way to look inside your colon, and in some instances, treats the problem. It should not be associated with looking for cancers only.
It is important to check with your doctor regarding the various risk factors and get advice on the procedure. Remember, it is never too early to check for pre-cancer symptoms as when it comes to cancer! Speed is key.
Commonly, we investigate a patient for bleeding from piles (haemorrhoids), only to discover cancer in the colon (which had no symptoms).
This explains why your doctor might advise you for a colonoscopy even if it seems like the source of the bleeding is likely to be from your anus, especially in the presence of risk factors or being in the screening age group.
Where can you get a Colonoscopy in Singapore?
Colonoscopies are performed in both private and restructured hospitals, as well as endoscopy centres. The procedure can be performed by a colorectal surgeon, general surgeon, or gastroenterologist.
An initial clinic consult with the doctor is required to assess the need for colonoscopy as well as to ensure that there are no medical conditions that may be a contraindication to having a colonoscopy.
Duration of a Colonoscopy
The duration of a colonoscopy may differ based on the configuration of the patient’s colon and whether polyp removal is required. A scope generally takes about 20 to 30 minutes if no polyps are found.
If polypectomy (polyp removal) is performed, a longer duration of up to 1 to 2 hours may be required depending on the number of polyps found and their size.
Even when an extended duration is required, the procedure is relatively painless for patients as they are sedated throughout the length of the procedure.
What happens during a Colonoscopy in Singapore?
Before your colonoscopy, it is important that you inform your doctor if you are on any form of blood-thinning medications such as:
- Warfarin
- Aspirin
- Plavix
- Rivaroxaban
These medications increase the risk of bleeding during the colonoscopy and may need to be stopped prior to the procedure. If you are unsure, please do run through your medications with your doctor.
Bowel preparation or cleansing is required prior to colonoscopy to enable a good view of the colon without obstruction from faecal matter. There are several steps involved in this preparation.
- A diet low in fibre is usually advised for a few days before the colonoscopy.
- This is followed by a strong laxative either the evening before (if your colonoscopy appointment is in the morning), or on the morning of the procedure (if your appointment is in the afternoon).
- A liquid-only diet is recommended once you have consumed the laxative.
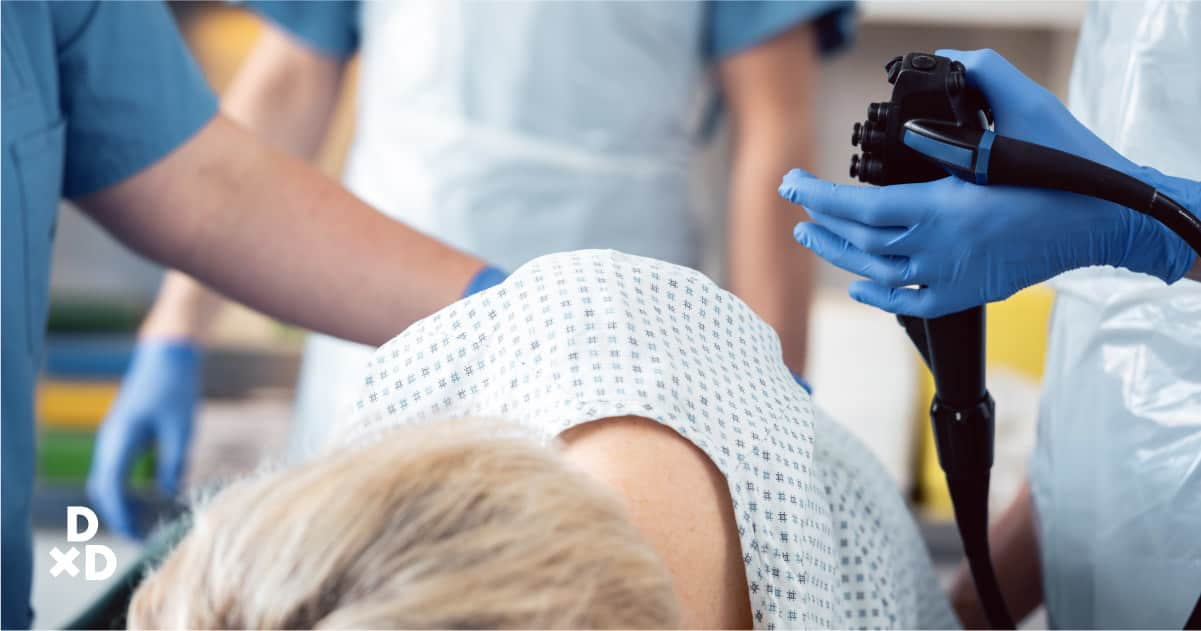
On the day of the procedure, the nurses will help to prepare you for the colonoscopy and will assist the surgeon during the procedure.
Sedation will be given intravenously (injected via the veins in your hands) before the procedure commences. Once the colonoscopy is completed, you will be brought to a recovery room where you can rest while the sedation slowly wears off.
You can usually be discharged from hospital within 1 to 2 hours. The results of the colonoscopy will be explained to you before your discharge, although histology reports from any biopsies or polyp removal will only be ready after 3 to 5 days. These will be disclosed to you at your next clinic visit with the doctor. [4].
What are some misconceptions about Colorectal Cancer?
Only older patients get cancer
One of the most common misconceptions is that colorectal cancer only affects older patients. This is untrue as 20-25% of colorectal cancer patients in Singapore are younger than 55 years old.
According to a study done at the National University Hospital which examined young colorectal cancer patients less than 50 years old, one-fifth of these young patients were diagnosed with stage 4 cancer. This means that the cancer has spread to organs outside the colon and survival rates are much poorer.
This indicates that not only can younger patients contract colorectal cancer, they can also be diagnosed with advanced cancer even at a young age.
I live a healthy lifestyle, hence I won't get cancer
Another common mistake is equating a healthy lifestyle to zero or low chances of having cancer. While it is true that a healthy lifestyle may reduce the chances of getting cancer, there are numerous cases of patients being diagnosed with cancer even when they believe that they live perfectly healthy lives.
This is because cancer is a complex disease with many factors contributing to its development, of which lifestyle is only one of them.
I won’t get cancer because there is no history of cancer in my family
Although having a family history of colorectal cancer increases an individual’s risk, having zero family history of cancer does not mean one is safe. Although cancer is genetic, about 80% of colorectal cancer patients do not have a family history of the disease.
If I don't have any symptoms, I do not need to go for tests
The lack of symptoms does not mean you should not go for routine checkups. Screening refers to doing a test to check for any diseases even when there are no symptoms.
The reason for recommending screening is because precancerous polyps and early stages of colorectal cancer are often not associated with any symptoms. Once an individual becomes symptomatic, the disease is often in the more advanced stages.
Hence the need to perform screening to diagnose the disease at an earlier stage when treatment is more likely to result in full recovery.
Why do people avoid Colonoscopies?
"I have no symptoms"
One of the main reasons why people avoid colonoscopies is because they have no symptoms and hence do not feel the need to go for any tests.
However, as mentioned above, polyps and early-stage colorectal cancer often do not manifest any symptoms. Hence it is imperative to go for screening once you reach the recommended age.
"Fear of pain during the procedure"
The thought of having a tube inserted via the anus incites fear in most people. However, as sedation is given throughout the procedure, minimal or no pain should be experienced from a colonoscopy.
"Bowel preparation is too much work"
There is a need for a special diet and consumption of strong laxatives prior to a colonoscopy. Furthermore, the laxatives lead to diarrhoea which may cause some mild discomfort. These cause people to shun away from colonoscopies as some feel that it is too much work to prepare for a medical procedure.
How painful is the Colonoscopy procedure?
I understand what most people think: a colonoscopy is uncomfortable. But that's mainly due to the distension (enlargement) of the colon. This results from the air pumped into the colon, as well as the sensation of the colonoscope inside the intestines.
However, as most patients undergo the procedure with sedation, you will likely sleep through the whole procedure without much recollection.
Most patients do not experience any discomfort after the procedure once they have passed the air out.

Are there any trends in Colonoscopies in Singapore?
From my experience as a doctor, there is an increased awareness of colorectal cancer and the need to go for a colonoscopy in Singapore.
However, a study performed in Singapore a few years ago indicated that although people were aware of the need for colon cancer screening, the majority had not gone for screening even though they were in the appropriate age group for screening.
The reasons given included not having time and not having symptoms.
It is obvious that more community education is required to increase the awareness of colorectal cancer screening in our population.
After the Procedure
If your colonoscopy is normal, then congratulations! An average risk individual who has a normal result will only require a repeat colonoscopy in 5 to 10 years time.
If polyps were found and removed, and histology reports confirm that the polyps were benign, it is recommended that you have a repeat colonoscopy in 3 to 5 years time.
Your doctor will advise you on the exact interval depending on the size and number of polyps found.
If you were unfortunately found to have a cancer, the doctor will advise you to perform more tests like a CT scan and blood tumour markers. This will allow the doctor to understand how advanced your cancer is and advise the next step of treatment.
The mainstay of colorectal cancer treatment is surgery, by removing the segment of the affected bowel. Patients with more advanced cancer may require chemotherapy and/or radiotherapy.
Conclusion
it is important to note that a colonoscopy is 95-98% accurate with good bowel preparation. This is because small lesions can hide behind the folds of the colon such that they go undetected during the examination, leading to some false negatives.
As the false negative rates are fairly low, colonoscopies remain the gold standard for colonic evaluations.
Regular colonscopies can prevent colorectal cancer. With plenty of private and restructured hospitals offering this service, please go for colorectal cancer screening. Prevention is always better than cure. I always tell my patients, family and friends: check early, you never know when it may save your life!
I hope this article has helped to dispel some myths and unwarranted fears about undergoing a colonoscopy.
With an abundance of endoscopy facilities available now, speak to your regular doctor about screening for colorectal cancer. Screening saves lives.
If you are looking to reach out to a doctor for treatments, you may do so here.













